|
Malignant "behavior" refers to cells that have lost the ability to contribute to the well-being of the host.
Cancer cells begin as normal cells. Damage to DNA causes the cells to lose growth or survival controls. The cancer cells live too long and/or divide too rapidly.
Cancer cells are frozen at a stage of development - they are unable to differentiate or have a normal life span.
Understanding the basic concepts of DNA and genes is not difficult and it can help you to appreciate current directions in clinical research. Click here for a summary explanation.
Related Items
* Andrew Wolf: Mutations in cancer 
* Andrew Wolf: On tumor suppressor genes 
* Upworthy 2014: 
Everything you Wanted to Know About Cancer But Your Doctor Was Too Busy To Tell You
*Huff Post 2014;
Your Cancer Is Not My Cancer: The Danger of Comparison http://huff.to/1i9r6gF
SNIP: I remind myself that I cannot compare my cancer to anyone else's cancer, even those who appear to have the exact same diagnosis and staging as mine. Their cancer is not my cancer. Their outcome is not my outcome. And no good will come of allowing myself to go down the mental rabbit hole of projecting someone else's outcome onto my future.
Not recognizing this is also what leads to promotions by patients for an approach that seemed to help them. The misguided reasoning goes: this worked for me ... so now I must convert others to the survival strategy I used so they can be helped too.
The scientific jargon for the variation in the biology and behavior found in same type of lymphoma is disease heterogeneity.
|
About Lymphoma > What is Lymphoma?
Last update: 08/10/2014
|
TOPICS
Lymphoma - general | Where Lymphoma develops | B-cells & T-cells |
Characteristics of b-cell Lymphomas - Stage & Grade |
WHO & REAL Classification Systems | Host/Tumor Interactions
Also see Lymphoma simplified
|
What is Cancer?
________________________
Cancer cells are also
called malignant cells
|
Lymphoma is a type of cancer.
Cancer cells are the descendants of a single normal cell in which genetic errors, or mutations, have occurred. These errors cause the cancer cells to over- or under-produce proteins that abnormally affect the cell's behavior - causing these cells divide too fast or fail to die when they should.
Cancer cells are typically clonal meaning that the descendent cells share the defects of the parent cell, but they can acquire additional mutations.
The malignant behavior, such as how aggressive or slow growing it might be, is determined by the cell type, the kinds of mutations, and sometimes the host environment.
There are as many kinds of cancers as there are cell types: skin, lung cancer, and blood cell cancers, etc.
In cells, genetic errors occur in the basic building blocks of DNA called genes. These errors might occur randomly when the cell divides, or they may result from exposure to environmental toxins called carcinogens - meaning able to cause cancer - but also from chronic inflammation or infection.
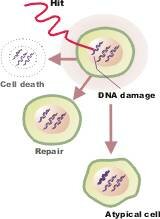 Normally the damage that can lead to cancer is detected and addressed: Normally the damage that can lead to cancer is detected and addressed:
When a cell detects errors within itself it can sometimes make repairs.
If the cell cannot repair the errors, a secondary safeguard can be executed by the cell called apoptosis. The damaged cell sacrifices itself for the good of the body by committing suicide.
The immune system can also recognize damage cells - cells that express abnormal proteins - and kill them before tumors can form and cause problems.
So cancers are not thought to be the result of a single event. A combination of negative events and missed opportunities are probably required.
When a malignant cell does form, it eventually reproduces to create a collection of cancer cells called a tumor. This mass can interfere with the proper functioning of the body.
|
Lymphoma is
a group of
related cancers
Download our
What's Lymphoma brochure PDF
|
Lymphoma is not one cancer, but a name for a group of related cancers that arise when a Lymphocyte (a blood cell) becomes malignant.
The normal function of lymphocytes is to defend the body against pathogens and infected cells: germs, viruses, fungi, even cancer. There are many subtypes and maturation stages of lymphocytes and therefore there are many kinds of lymphomas. When a lymphocyte becomes malignant (goes bad), it's biologic behavior is arrested at that stage.
"Malignant lymphomas represent clonal malignancies in which the majority of cells are frozen at a single stage of normal lymphocyte differentiation" Source: Norman Levy, MD - Lecture
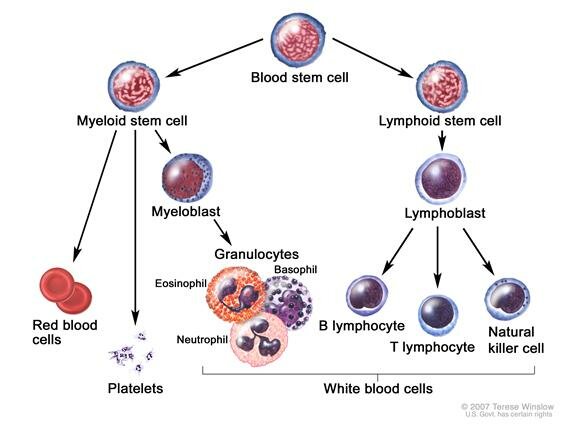
Source http://www.cancer.gov | full image
|
Where Lymphoma
develops
STAGING
Extranodal means 'beyond nodal' - sites are identified by the following notation:
| N |
= lymph nodes |
| E |
= extranodal |
| H |
= liver (hepatic) |
| L |
= lung |
| M |
= bone marrow |
| S |
= spleen |
| P |
= pleura (lung) |
| O |
= bone |
| D |
= skin (dermis) |
Also see Musshoff - classification of gastrointestinal lymphomas
|
Like normal cells, malignant lymphocytes can move to many parts of the body. Typically, lymphoma cells form tumors in the lymphatic system: bone marrow, lymph nodes, spleen, and blood. However, these cells can migrate to other organs.
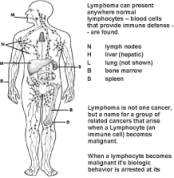
Lymphoma Sites of Presentation.
Click image to enlarge it.
Certain types of lymphoma will tend to grow in locations in which the normal version of the cell resides. For example, it's common for follicular NHL tumors to develop in the lymph nodes. MALT lymphomas will manifest in other areas as described here:
"Lymphoid tissue in the human body is associated with the mucosal system. This tissue, mucosa-associated lymphoid tissue (MALT), is scattered along mucosal linings and protects the body from antigens entering along mucosal surfaces." - emedicine
|
The maturation stage of the cell of origin determines the type of lymphoma
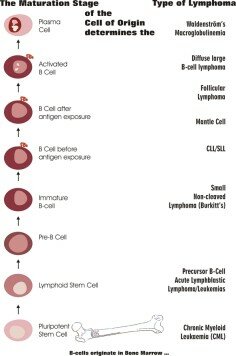
Click image to enlarge
|
Normal lymphocytes are part of a group of cells called white blood cells. There are two main kinds of lymphocytes.
.gif) |
B-cells originate and mature (differentiate) in the bone marrow.
|
.gif) |
T-cells also start out in the bone marrow, but they differentiate and mature in the thymus gland.
|
Natural Killer cells are a third kind of lymphocyte. They specialize in killing foreign cells and possibly signaling to alert other immune cells of invaders.
Two broad types of lymphoma are T-cell and b-cell lymphoma. We will focus mainly on the b-cell lymphomas in this text.
Hodgkin's disease describes a cancer of a unique malignant cells known as Reed-Sternberg cells. It is not as common as Non-Hodgkin’s Lymphoma. Fortunately, Hodgkin's disease is considered curable in many cases.
B-cells originate from stem cells in the bone marrow. They then mature and migrate to different parts of the body and perform unique functions at each stage. The developmental stage of the b-cell when it becomes malignant determines the specific kind of lymphoma.
For example, follicular, large cell and immunoblastic Lymphomas result when a malignancy develops after a b-cell has been exposed to antigens (bacteria, virus etc.), while CLL and SLL malignancy develop when a mutation occurs prior to antigen exposure. See the illustration on the left.
What makes one lymphoma aggressive and the other indolent? The cell type, the type of damage within the cell, and level of maturation (stage of development) of the cell when it became malignant are few reasons. For example, just as children grow faster than adults, cells at various stages of development grow faster than at other stages.
When a cell becomes malignant its maturation stage is arrested (stopped) at that stage, and it's behavior (fast growing, refusing to die) is therefore determined in part by the level of maturation of the cell of origin.
|
Characteristics of Lymphomas
Extranodal (beyond nodal) sites are identified by the following notation:
N = lymph nodes
H = liver (hepatic)
L = lung
M = bone marrow
S = spleen
P = pleura (lung)
O = bone
D = skin (dermis)
Disease Staging may also be accompanied by local involvement of an extranodal organ or site, such as the spleen (IIIS).
ANN ARBOR STAGING
further classifies patients with NHL into A or B categories:
A = without symptoms
B = with symptoms including unexplained weight loss (10% in 6 months prior to diagnosis, unexplained fever, and drenching night sweats.
STAGE IV: It is common for b-cell lymphomas to be diagnosed at stage IV, which includes bone marrow involvement. Please note that successful treatment is often possible for stage IV disease and bone marrow involvement is reversible.
|
Characteristics of B-Cell Lymphomas
.gif) |
Cell type are primarily determined by Histology - The size; nuclear and cellular features of lymphoma cells allow for the identification of the lymphoma by its appearance and its markers. (See WHO and REAL classification systems below)
|
.gif) |
Pattern (follicular or diffuse) - The pattern by which a lymphoma infiltrates and replaces a previously normal lymph node is predictive of its biological behavior. The architectural pattern of the proliferating process, that of either a diffuse or a follicular appearance, is of prognostic value - in general follicular pattern has a better prognosis than diffuse pattern.
|
.gif) |
Grading defines how aggressive or slow growing the malignant cells are likely to be. This is sometimes called histologic grade, which is determined by the appearance of cells under the microscope:
.gif) |
low grade or indolent
.gif) |
Grade 1 = small cell
|
.gif) |
Grade 2 = mixed small and large cell
|
Note: both grade 1 & 2 can behave similarly.
The determination of these grades can depend on the sample evaluated under the microscope.
Sometimes grades of indolent lymphoma are subdivided in this way:
.gif) |
A. Small lymphocytic
|
.gif) |
B. Follicular, predominantly small cleaved cell
|
.gif) |
C. Follicular mixed, small and large cell
|
Also see Grade
|
|
.gif) |
intermediate- or high-grade
(today these are both often referred to as aggressive).
|
.gif) |
Staging defines how widespread the disease is and the locations of the disease in the body. * See Extranodal and Ann Arbor Staging codes in left column, which may be added to the staging designations.
|

Click the image to enlarge it.
Anne Arbor staging for Hodgkin's disease - Virginia.edu
.gif) |
Stage I disease in single lymph node or lymph node region.
|
.gif) |
Stage II disease in two or more lymph node regions on same
side of diaphragm.
|
.gif) |
Stage III disease in lymph node regions on both sides of the
diaphragm are affected.
|
.gif) |
Stage IV disease is wide spread, including multiple involvement at
one or more extranodal (sites such as the bone marrow).
|
Also see Staging - Oncologychannel.com | Stage
"The prognosis and treatment of lymphomas is based on
- The dominant cell type (and it's inherent biologic behavior)
- The extent of spread (Stage) and
- The underlying health of the patient
Source: Norman Levy, MD - Lecture
|
B-Cell Non-Hodgkin's Lymphoma in the WHO Classification System
WHO utilizes morphologic differences in cells.
Morphologic - appearance
or structure
Source: The Who's WHO in Lymphoma
.gif) |
Salient cytogenetic entities Antonio Cuneo
|
.gif) |
WHO Classification of B-cell Lymphoid Neoplasms - World Health Organization Classification of Neoplastic Diseases
|
|
WHO CLASSIFICATION SYSTEM FOR B-CELL LYMPHOMAS
.gif) |
Small lymphocytic lymphoma (SLL/CLL)
|
.gif) |
Mantle cell lymphoma (MCL)
|
.gif) |
Follicular lymphoma (FL)
|
.gif) |
Marginal zone lymphoma (MZL)
|
.gif) |
Extranodal (MALT lymphoma)
|
.gif) |
Nodal (Monocytoid B-cell lymphoma)
|
.gif) |
Splenic
|
.gif) |
Diffuse large cell lymphoma
|
.gif) |
Burkitt's lymphoma
|
.gif) |
Lymphoblastic lymphoma
|
|
B-Cell Non-Hodgkin's Lymphoma in the REAL Classification System
The REAL system utilizes morphologic, immunophenotypic, and genotypic differences in cells.
Morphologic - appearance or structure
Immuno - pertaining to immune cells.
Phenotype - observed properties or outward appearance of a trait or expression of proteins. CDs are expressed on immune cells depending on their maturation. Identifying these CDs (clusters of differentiation) that appear in immune cells helps to identify immunophenotypic differences.
Genotype - a cell's genetic composition.
Phenotype - results from the interaction of the genotype with the environment.
|
REAL CLASSIFICATION SYSTEM FOR B-CELL LYMPHOMAS
.gif) |
Small lymphocytic lymphoma (SLL/CLL)
|
.gif) |
Mantle cell lymphoma (MCL)
|
.gif) |
Follicular lymphoma (FL)
|
.gif) |
Marginal zone lymphoma (MZL)
.gif) |
Extranodal (MALT lymphoma)
|
.gif) |
Nodal (Monocytoid B-cell lymphoma)
|
.gif) |
Splenic
|
|
.gif) |
Diffuse large cell lymphoma
|
.gif) |
Burkitt's lymphoma
|
.gif) |
High grade Burkitt-like lymphoma
|
.gif) |
Lymphoblastic lymphoma
|
|
Host/tumor interactions: the microenvironment
angiogenesis
immune system
cytokines
growth factors
|
Scientists are working to understand how the body interacts with malignant cells to restrain and/or promote the growth of tumors. Malignant cells don't exist in a vacuum. They may interact with the body in normal, near-normal, or dysfunctional ways.
Angiogenesis: As b-cell tumors grow, they form microvessels, presumably to obtain oxygen and nutrition from the blood supply. Hypoxic (low oxygen) conditions can induce malignant cells to over express genes that promote angiogenesis-the process in which cells recruit the formation of a blood supply by secreting vascular (blood) growth factors.
Immune system: There is evidence that the immune system can fight lymphoma and inhibit it's progression in some cases. Immune cells use cytokines and cytokine receptors to send and receive messages. These complex interactions can be positive or negative in respect to progression of the disease.
Self-stimulation: Malignant cells can acquire additional mutations that can cause them to become self-stimulating. For example, a malignant cell could express a growth factor that causes itself to grow faster.
Cytokine stimulation: Inflammatory and growth stimulation may develop from dysfunctional interactions with other immune cells that may express (give off) protein messages called cytokines (such as IL-6), that may promote the growth of malignant lymphocytes.
Antigen stimulation: Some b-cell cancers, such as follicular NHL, are antigen driven. That is they are activated like normal b-cells to divide by the presence of antigens (allergens, bacteria, etc.) in the body. Malignant cells may act normally in this regard, but one or more genetic defects prevents them from dying when their work is done. Thus, malignant b-cells are often said to be immortal.
RELATED ABSTRACTS
-
Chronic B cell malignancies and bone marrow microenvironment.
Semin Cancer Biol. 2002 Apr;12(2):149-55. Review. PMID: 12027587- PubMed
-
The indispensable role of microenvironment in the natural history of low-grade B-cell neoplasms. Adv Cancer Res. 2000;79:157-73. Review. PMID: 10818680 PubMed | Related Abstracts
-
CXCL13 (BCA-1) is produced by follicular lymphoma cells: role in the accumulation of malignant B cells. Br J Haematol. 2002 Nov;119(2):492-5. PMID: 12406091 PubMed
-
Scientists Unlocking Lymphoma's Secrets - The microenvironment healthscout.com 2004
"Genetic differences -- not in lymphoma cells, but in immune cells surrounding the tumor -- may determine how aggressive a particular case of follicular lymphoma turns out to be"
-
How do follicular dendritic cells interact intimately with B cells in the germinal centre? Microenvironment connection to lymphoma: "Follicular Dendritic cells (FDCs) prevent apoptosis of germinal centre B cells and stimulate cellular interaction and proliferation." ochsner.org PDF
|
|