|
TOPICS
Bias | Associations: Causal or Coincidental? | Subset analysis?
Baseball & the FDA | Billiards and Clinical trials: Retrospective versus Prospective | Hazard Ratio? | Odds Ratio | Relative Risk?
Identifying Quackery | Is there an Impartial group? | Terminology | Statistics | Types of clinical data (best first)
The Problems with Testimonials
Weighing Sources of Medical Evidence | References
Common Myths About Cancer | When Laypersons give medical advice
 Observations can fool us, as described in this historic example: Observations can fool us, as described in this historic example:
"For many centuries doctors used leeches and lancets to relieve patients of their blood. They knew that bloodletting worked. EVERYBODY said it did. When you had a fever and the doctor bled you, you got better. EVERYONE knew of a friend or relative who had been at death’s door until bloodletting cured him. Doctors could recount thousands of successful cases."
Why We Need Science: “I saw it with my own eyes” Is Not Enough
Without standards for testing treatment ideas,
we'd have thousands of choices with no basis for making a helpful choice,
and no foundation on which to make reliable scientific or clinical progress
The importance of trying to see things as they are:
... and knowing what we do not know.
Our goal is to help patients and caregivers to weigh the strengths and weaknesses of medical claims and reports.
We encourage patients and caregivers to develop the good habit of asking informed questions. If a study finding is strong the authors will be able to provide good answers and will be happy to do so. Do the results reported predict outcomes in the real world ... predict what will happen to me or you? Was everything that is important to report (clinically relevant), provided in the abstract or the press release?
How do we start?
By focusing on the methods of the study, not just the results and the conclusions of the authors.
By learning about the key factors that can influence how the study is interpreted, such as:
How many participated in the study (1, 6, 30, 50, or 300)?
How were the participants selected?
(type of lymphoma, eligibility: age, exclusions, prior treatments, etc.)
Was there a control group?
What is the natural history of the disease for the eligible participants?
(varied, predictable, favorable, short survival without treatment?)
How were the treatment effects (good and bad) measured?
What was the length of follow up?
(did the effects last, were there late bad effects?)
By reviewing the source document, instead of the press release
By recognizing the potential influence of conflict of interest
By asking if other groups have had similar findings in similar populations
By asking independent experts in the field
Return
Bias: different reasons for different groups:
"Bias" has two meaning:
(1) "an inclination of temperament or outlook; especially: a personal and sometimes unreasoned judgment." Bias can influence how one looks at outcomes, or in what we choose to read or ignore.
(2) In a study design, a bias is defined as an error in the method of study that leads to a deviation in the outcome away from the truth.
Sources of Bias:
Financial conflict of interest
Wikipedia: "A conflict of interest is a situation in which someone in a position of trust, such as a lawyer, insurance adjuster, executive or director of a corporation or a medical research scientist or physician, has competing professional or personal interests. Such competing interests can make it difficult to fulfill his or her duties impartially. A conflict of interest exists even if no unethical or improper act results from it. A conflict of interest can create an appearance of impropriety that can undermine confidence in the person, profession, or court system."
Conflicts of interest occur when personal, professional, or financial interests intentionally or unintentionally influence decisions on scientific methods, or how data from the study are interpreted.
"A financial conflict of interest, I believe, is any financial association that would cause an investigator to prefer one outcome of his research to another. Let me give you an example. If an investigator is comparing drug A with drug B and owns a large amount of stock in the company that makes drug A, he will prefer to find that drug A is better than drug B. That is a conflict of interest." ~ Marcia Angell, M. D. Source: ohrp.osophs.dhhs.gov
Those who develop new drugs or sell supplements have an inherent financial conflict of interest with respect to objectively evaluating the true worth and benefits of their products or services, which can lead to selective reporting or "hyping" the products in order to maximize shareholder confidence and the profitability of the company that sells them.
Scientists who have financial interests in products or services must disclose these relationships, which make them inherently less able to overcome the biases these monetary interests can create.
"While most people think conflicts of interest are a problem of overt corruption, that is, that professionals consciously and intentionally misrepresent the advice they give so as to secure personal gain, considerable research suggests that bias is more frequently the result of motivational processes that are unintentional and unconscious " 4
Consider that, by investing in a company, a scientist may demonstrate a belief in the value of its product, perhaps in advance of evidence. Scientists have an ethical responsibility to avoid arriving at conclusions ahead of time. The discipline of science requires that theories be tested in well-controlled studies, and that the outcomes be evaluated objectively before conclusions are made.
ASK:
- "Was as the research funded by an organization that generally advocates a specific point of view?
- Do the findings of the research parallel the organization's point of view - or too closely?" 2
Reporting bias:
Because of personal inclinations, expectations, or other biases, a participant in a study may report events more favorable to the hypothesis, and leave out, or not see, events that contradict it. There is also the potential for this type of bias in case reports
Selection bias:
Investigators may introduce bias into a study by selecting patients who have characteristics (such as young age) that are favorable to a desired outcome; and also by excluding patients who do not (such as patients with low blood counts). Randomized studies protect against this kind of bias.
ASK:
- Was the data source manipulated to produce analyzable data?
- Was the data source selected with an unusual methodology?
- Was the data source unusually small or narrow, or tightly controlled by the researcher?
- Was the data source self-selected (not random)?
Intellectual/confirmation bias:
Investigators and scientists can develop unintended prejudices about the value of their own work, ideas, or intellectual property.
Investigators may unconsciously see benefit when none exists, or they may set up a study in ways more likely to reveal weaknesses, exaggerate the benefits, overlook unanticipated side effects, and so on.
I know that most men, including those at ease with problems of the greatest complexity, can seldom accept even the simplest and most obvious truth if it be such as would oblige them to admit the falsity of conclusions which they have delighted in explaining to colleagues, which they have proudly taught to others, and which they have woven, thread by thread, into the fabric of their lives.”
~ Leo Tolstoy
ASK:
- Is the researcher affiliated with an organization that promotes a specific point of view?
- Does the researcher produce studies that consistently generate the same conclusions? 2
- Is the research group the ONLY group interested in the research question?
Confirmation bias is the tendency to give more weight to incidents and data that conform to preexisting beliefs and to forget things that do not.
"We're all prone to it, including scientists. One major advantage of the scientific method is that it is pretty good at overcoming confirmation bias." Source: http://scienceblogs.com
Biases common to patients and caregivers:
Denial: In order to cope with living with a life-threatening disease, patients or caregivers may develop a tendency to minimize the dangers of the disease, or to inflate the potential of alternative and other less toxic approaches to control it. Denial can lead to missed opportunities and delays that can make the disease more difficult to treat.
Fear: To be fearful of a cancer or cancer treatment is to be human, and sometimes it's justified. In patients, the fear of the toxicity associated with many standard cancer therapies can form a bias in favor of claims made for safer alternative, or even investigational low-toxic therapies.
We are highly prone to wishful thinking.
Physician biases (reasons to consult independent experts):
Even a trained oncologist can have conflicts of interest, biases, or gaps in knowledge - especially if he or she does not specialize in lymphomas.
Investigators may have intellectual biases about any therapies they may be testing.
Community doctors might have biases in favor of what is easiest to administer.
HMO physicians may prescribe what is least expensive. Other doctors might be influenced, perhaps unconsciously, by sales promotions from the drug industry.
Patients expressing their desire to continue working without interruption may influence a busy physician to prescribe what meets the immediate needs, without fully discussing possible negative long-term implications of that treatment decision.
References and Further Reading:
1. For a readable and concise paper on scientific integrity ethics.ucsd.edu
2. Potential Sources of Bias ascd.org pdf
3. The Dirt on Coming Clean: Perverse Effects of Disclosing Conflicts of Interest cbdr.cmu.edu .pdf
4. Identifying Your Biases: wpas-rights.org
"It is important to recognize your biases, and to periodically evaluate whether they are interfering with your judgment. The first step to not letting bias interfere with your judgment is to accept that it's there and decide to deal with it."
Associations: Cause and Effect?
Did an action lead to an outcome? ... or was it coincidental?
An association is an observation that one event or condition occurs with another. But associations do not mean one thing caused another. That is, associations do not prove causality - the relating of causes to the effects they produce.
Example A:
Suppose a survey shows that that people who drink wine live longer than those who drink beer.
We might be tempted to interpret this association to mean wine is better for you than beer. However, it may be that people who choose wines are more likely to eat healthier foods, or that foods that go well with wine are better for you than foods that go well with beer.
So the chips and pizza are confounding variables and the study does not yet prove causality: the consumption of wine might not influence health one way or the other.
Example B:
There's a likely association between people who wear crash helmets and brain injury.
However, it's easy to recognize it's the high-risk activities of folks who must wear helmets that increase risk of brain injury, not the helmets.
Example C:
In any study, better outcomes may be observed for people born in August or January.
The last example obviously explained by chance.
Forming conclusions that A caused B can range from harmless to dangerous:
Harmless, when a baseball player hits a home run and recalls that he had eggs for breakfast that day - who then continues to have eggs on game days.
Dangerous, when a patient delays a needed treatment based on anecdotal reports (an association taken as fact) that use of an herb can control the disease.
However, observations and exploring possible connections between events (forming hypothesis) is the starting point of science - inspiring further research and well-controlled experiments that prove or disprove it.
Since random associations are so common, plausibility is required before expensive research would be done. For example, it would be foolish to study the effects of birth dates on outcomes, or to test if minute fractions of a compound - too small to measure - could have therapeutic effects on human disease. See Homeopathy discussion.
Here are some common assumptions about cause and effect related to indolent lymphoma, kept alive by testimonials:
.gif) |
My disease is stable, therefore the life style changes I have made are helping.1
|
.gif) |
|
.gif) |
A drug resistance assay predicted my response to treatment and my response was great. Therefore,
the assay is proven to be valid. 2
|
.gif) |
|
.gif) |
My lymph nodes are regressing, therefore the investigational vaccine I took is effective.2
|
.gif) |
|
.gif) |
My lymph nodes started growing after I had chocolates, therefore chocolate cause progression.1
|
.gif) |
|
.gif) |
My lymph nodes started regressing while taking Aloe Vera, therefore it's effective against the disease.1
|
1 Patients with indolent lymphomas may be particularly susceptible to confusing cause and effect, because the natural course of the disease is so variable. It may remain stable for many years without any intervention, or regress spontaneously "as many as 20% to 30% of patients will experience regressions at some time in the clinical course of their disease."
Therefore, if a practitioner prescribes a life style or alternative protocol that 100 patients follow, as many as 30% are likely to do well because they would have done well anyway. This "effect," - which has good probability of being unrelated to the practice - will often result in strong belief and promotions, as in: "How can you argue with my success?"
2 Lymphoma is sensitive to many treatments and has a variable natural course - can wax and wane independent of therapy. The proof that an assay can predict response would therefore require controlled studies on many patients over time.
Practitioners have an obligation to state that their ideas and practices have not been proven to provide benefit or predict outcomes.
Vaccines and Autism link:
It's easy to confuse correlation with causation, by Tony L. Hines
Regarding preliminary scientific reports:
John Godfrey Saxe's version of an Indian parable applies to the quest for understanding - and actually understates the complexity of human biology and drug interactions, thousands-fold.
It was six men of Indostan
To learning much inclined,
Who went to see the Elephant
(Though all of them were blind),
That each by observation
Might satisfy his mind.
The First approached the Elephant,
And happening to fall
Against his broad and sturdy side,
At once began to bawl:
"God bless me! but the Elephant
Is very like a wall!"
... http://en.wikipedia.org/wiki/Blind_men_and_an_elephant
Subset analysis ... (a target shooting analogy)
Larry wrote:
The drug failed to achieve the primary goal(s)/ endpoints the researchers (and drug company) set for themselves ahead of the clinical trial.
By slicing and dicing the data after the fact, in a small subset of the patient cohort, they drew statistically iffy conclusions that served their argument.
As some wag once put it:
After-the-fact sub-set analysis is like shooting at a barn, then painting bulls-eye around the bullet hole, where ever it happened to be. ... Hardly compelling "proof".
Careful patient advocacy requires that we be able to tell the difference between
marketing hype of companies with clear financial interests and cases where
regulatory hurdles are keeping back a truly valuable drug from the patient
community.
The drug in question is hardly a good example for getting the patient community
mobilized.
.gif) |
Subset analysis - an example http://bit.ly/mwHalt
This subgroup analysis suggested that the treatment was quite effective and statistically significant for all patients except those born under the sign of Gemini or Libra. The difference in outcome with respect to astrologic sign was naturally an artifact and would not be reproducible in subsequent studies. This was the point of their analysis.
|
Baseball and the FDA:
Pitchers often believe every close pitch is a strike and that the strike zone is too small. So just as we recognize the need for a neutral party to call balls and strikes in baseball, we should also recognize the more urgent need for an impartial agency, such as the FDA, to evaluate claims of medical benefits and risks.
In order to test claims the drug sponsor must conduct well-designed studies that minimize bias and demonstrate safety and efficacy for a given condition. Absent evidence-based tests and assessments we'd return to a "Wild West" environment with no means of making informed or safe medical decisions, and no good foundation on which advances in clinical science could be made.
Is the FDA without bias and conflict of interest?
No agency or human being is completely free of bias, but the agency is committed and mandated by law to achieve impartiality. There are strong policies on ethics and conflicts of interest in place, and criminal penalties can be invoked for violations of these regulations.
About FDA's Ethics Program: "The Agency’s ethics program is administered to help ensure that decisions made by Agency employees are not, nor appear to be, tainted by any question of conflict of interest. The "ethics" laws and regulations were established to promote and strengthen the public’s confidence in the integrity of the Federal Government. The Agency’s Ethics and Integrity Branch provides advice and assistance to FDA employees on a variety of ethics related matters including, but not limited to, financial disclosure, prohibited financial interests, outside activities, co-sponsorship agreements, and post employment."
See FDA.gov/opacom/ethics/
Billiards and Clinical Trial Design:
Retrospective versus Prospective trial designs
There are two basic types of studies: retrospective and prospective. Understanding each can help the patient advocate to better converse with scientists on drug development and assessment ... and help consumers (all of us) to evaluate the strength of evidence in scientific reports, and other medical claims.
A patient advocate provided a nice analogy to help compare retrospective and prospective studies:
"Shoot a cue ball into a pack of billiard balls and the 7 ball goes in the side pocket. A retrospective analysis *looks back* at the shot with the objective of finding evidence that guides how to play pool to win. The prospective study, on the other hand, starts with a hypothesis and tests it going forward: "I will shoot the ball into the pack this way, and I predict the 7 ball will go in the side pocket." So with a prospective study you must call your shot in advance.
Thus, the prospective study provides a much higher level of confidence that the outcome was determined by the action (that is was causal), and can be repeated ... that it was not the result of chance or other factors.
Is the results of a single prospective experiment sufficient evidence? Generally not, unless the findings are "robust." Most often a second experiment will be needed to validate the first. You also want to scrutinize the DESIGN of the experiment to see if it contains BIASES (study flaws) that may have "rigged" the outcome. ... Perhaps the 7-ball was put near the side pocket, or the table slants that way.
An example of bias in a clinical trial is when investigators select "ideal" patients that have a favorable prognosis (good counts, young age) ... or they don't count participants in the analysis who died from "unrelated" causes, or they do not give sufficient weight to side effects ...
The main purpose of doing controlled experiments is to achieve an acceptable LEVEL OF CONFIDENCE that the positive effects measured in the experiment predicts what will happen to patients in the real world. The alternative to this expensive process is to rely on OPINION ... a return to the dark ages.
Importantly, there is never absolute certainty in these matters. Statistics is about measuring the level of certainty that an outcome in an experiment predicts outcomes for the rest of us ... so that we can have confidence that making a new drug available for an indication (cancer, diabetes, osteoporosis) is on balance better for the patients afflicted with the disease than no treatment, or an existing treatment.
So the billiard table analogy is useful but it oversimplifies. A clinical trial is many times more complicated. For example: what is the outcome that you are measuring (the end point), and how well does it predict clinical benefit? Does tumor shrinkage increase survival, or outweigh the risk bone marrow toxicity? Does an increase in time to progression offset the long-term risk of secondary MDS? Does the intervention improve overall survival or quality of life? Thus, the indication (cancer versus a cold), and what's already available to treat it, has a lot to do with how much risk is acceptable for the new drug.
Not surprisingly the drug sponsor will have a bias, because they are driven to do this difficult work in order to realize a profit. So the industry is prone to setting up, interpreting, and reporting on the experiment in ways that favor the benefit side of the equation.
Please note, however, that the PROFIT motive is ESSENTIAL to the process and to progress Without it new drugs would NEVER be developed or tested. We need all of these: the profit incentive, rigorous scientific method (controlled prospective studies), patient participation, and independent and impartial FDA review.
The barometer that we are heading in the right direction in general is an increase in life expectancy, and overall survival (OS) for various indications: Note the recent improvements in OS for indolent follicular NHL.
The purpose of conducting well-design trials is to avoid the many dangers of practicing medicine based on opinion. We want to be sure that an intervention - for a specific condition - provides clinical benefit. ...
For example, without use of a controlled study, Hormone Replacement Therapy (HRT) would still be a common practice today ... and, contrary to what was anticipated based on case observation and theories, we would still be giving these hormones to women, increasing the risk of heart disease and cancers.
Finally, importantly, with opinion-based medicine we would have no scientific foundation to build on. With the value of drug A based on opinion (observations and theory), we could not reliably compare it to drug B, or evaluate how prudent it is to test drug C with drug A.
Take away standards for approval -- as the Abigail Alliance appears to advocate for -- we would soon be victimized by claims, counterclaims, sales pitches, and promotions of inadequately tested drugs. Drugs would be released into the market with insufficient safety and efficacy information. Gathering this information is very much more difficult after marketing - and that absent standards of evidence for the release of new drugs, the difficulty would increase exponentially.
Is anyone's perspective more believable?
Perhaps we can learn quickly from the perspectives of doctors and scientists who have cancer, as the threatening nature of the disease is likely to remove any financial biases they may have had in respect to the integrity of the drug evaluation system in America.
"Patients who don’t understand the difference between information based on theory, anecdote, historical analysis, or double-blind placebo controlled studies are making ill-informed decisions, believing alternative therapies are safer or more effective when they are not.
Even patients who presume that alternative therapies are ineffective may use them. Why? When faced with a life-threatening disease requiring highly toxic treatments with no guarantees, or when dying because there are no effective conventional treatments, it takes guts to reject something or someone claiming to be able to save you, just in case you might be wrong." - Wendy S. Harpham, MD (NHL survivor) Full text: amcancersoc.org
Conspiracy theories are often used to promote unorthodox therapies
Please consider that such a conspiracy would require the complicity of many thousands of scientists, doctors, and regulators - who also get cancer and spouses, parents, grandparents, children, and loved ones also get cancer.
Quackery and Charlatanism:
Patients with lymphoma are particularly vulnerable to believing in easy, risk-free remedies.
The charlatan or quack has a message that appeals to wishful thinking and also our desire for certainty, which is an easy message to craft when unencumbered by the truth ... or an objective test that a theory actually works and provides clinical benefit.
In medicine - as in life - benefit is not often achievable without risk, and outcomes are rarely certain. Unlike the charlatan, the trained doctor is obligated to provide accurate information that is based on published clinical studies, which will describe both risks and benefits, relative to the disease untreated or treated differently.
Red flags of quackery:
See also our printable Red Flags and Free Speech PDF
|
|
It provides certainty that you will be helped or cured
|
|
|
Its promoted as a cure for many types of disease.
|
|
|
It's promoted solely by the practitioner.
|
|
|
The lack of acceptance of the promoted remedy is blamed on a conspiracy.
|
|
|
The remedy has no risks
|
|
|
The evidence is based entirely on testimonials
|
|
|
No clinical studies are cited.
|
Related Resources:
|
|
Charlatan, defined: wikipedia.org/
"A charlatan (also called swindler) is a person practicing quackery or some similar confidence trick in order to obtain money, fame or other advantages via some form of pretence or deception."
|
|
|
How Quackery Sells - quackwatch.org
"Most people think that quackery is easy to spot. Often it is not. Its promoters wear the cloak of science."
|
|
|
Helping Your Patients Deal with Questionable Cancer Treatments, William Jarvis, Ph.D.
caonline.amcancersoc.org pdf
|
|
|
On Charlatans and Quackery - grg.org
"Drs. Barrett and Herbert define a quack as anyone who fraudulently pretends to medical skills they do not possess. They distinguish among three types: dumb quacks (ignorant), deluded quacks (self-righteous, true believers), and lastly dishonest quacks "
|
|
|
What is Pseudoscience? - sciencethinking.com
The term pseudoscience can be applied to any information masquerading as science. The fakery may be obvious, as in the case of supermarket tabloids, or much more subtle, and potentially harmful, as is the case when well-known personalities recommend unproven remedies for serious medical conditions. What are some signs that can alert us to the presence of pseudoscience?
|
|
|
Traditional Medicine: Identifying Potential Cancer Treatments Of Herbal Origin http://www.sciencedaily.com
"ScienceDaily (Mar. 5, 2008) — Curing cancer with natural products -- a case for shamans and herbalists?
Not at all, for many chemotherapies to fight cancer applied in modern medicine are natural products or were developed on the basis of natural substances. Thus, taxanes used in prostate and breast cancer treatment are made from yew trees. The popular periwinkle plant, which grows along the ground of many front yards, is the source of vinca alkaloids that are effective, for example, against malignant lymphomas. The modern anti-cancer drugs topotecan and irinotecan are derived from a constituent of the Chinese Happy Tree."
|
Terminology to help you assess clinical data and medical claims:
"All scientific work is incomplete - whether it be observational or experimental.
All scientific work is liable to be upset or modified by advancing knowledge.
That does not confer upon us a freedom to ignore the knowledge
we already have or postpone the action that it appears to demand at a given time. "
- Sir Austin Bradford Hill (1965)
Abstracts | Theory | Treatment Response | Statistical Significance (p-value & confidence)
Abstracts:
Abstracts are summaries of larger papers and therefore do not contain all the available details of the study methods and data.
Abstract conclusions may not be accepted by experts in the field. Reputable peer-reviewed journals sometimes require modifications to conclusions from the original abstract for this reason -- or they may reject the paper from publication because it was determined that the methods (methodology) or data did not support the conclusions made in the abstract.
Therefore, it's important to avoid forming conclusions on the basis of abstracts. They should be considered only a starting point for discussions with your doctors and perhaps a basis for additional inquires and research.
Linda writes: "I think it's important to note that one must be very cautious in drawing conclusions from merely reading an abstract. It's important to read the full article, understand the methodology, and the strength of the statistics and research design to determine if the conclusions the authors present in the abstract are reasonable. The better the journal -- and the higher the quality of the peer review necessary to be published in the journal, the more likely the methods and design, etc. will be good. Even with that, I've seen some questionable studies get into good journals." - L - (NHL-survivor & medical professional)
Questions to ask:
1) Was the paper published in a respected journal?
2) What types of studies and methods were used to reach the conclusions?
3) Do papers published by other groups support the conclusions?
Reproducibility is valued in science, especially when a finding comes from a different investigative group. The reason for this is that it reduces the chance that bias, or choice of methods, or chance influenced the findings or the conclusions.
Key: start by asking questions of (not just accepting) the information we receive.
Theory (Hypothesis)
"A hypothesis consists either of a suggested explanation for a phenomenon (observable event or, quite literally, something that can be seen.)" wikipedia.org
Theories are starting points for experiments and studies. They should not be regarded as a proof, no matter the reputation of the author. When someone tells you that this is how a treatment works and that it is therefore desirable, you might ask:
What clinical data supports the theory?
Who published the findings, and in what journal?
Evidence-based medicine requires that a theory - the hypothesis - be tested objectively ...
in a way that minimizes biases - that the pool table is not tilted in a way that favors the theory.
Treatment response
Describes clinical outcomes from therapy based on a clinical change, such as the reduction in size of a lymph node. Responses, however, may or may not result in meaningful clinical benefit - defined as improved survival or the reduction of symptoms.
For example, with lymphatic cancers the lymph nodes can increase and decrease in size because of transient inflammatory reactions, which could lead to false assumptions about the benefit of a drug or a life style intervention. Also, the reduction in tumor size might be offset by the short or long-term toxicities of the drug.
Some questions to ask about response:
1) How long was the response?
2) At what intervals were the outcomes measured and with what tests?
3) Did the measured response correspond to clinical benefits?
4) Who reported the responses and were the outcomes verified by independent reviewers?
5) How large was the patient sample, and how were they selected?
6) What is the expected clinical course of the disease?
7) What were the short or long-term toxicities (the costs) relative to other treatments?
Mean (average), Median (middle), Mode (most common)
Mean (average) - the total of all numbers included divided by the quantity of numbers represented.
Median - the number midway through an odd set of numbers or
a value halfway between the two middle numbers in an even set.
Mode - the number or value that occurs most frequently in a series.
If two or more values occur with the same frequency, then you take the mean of the values.
Adapted from http://www.unc.edu/depts/wcweb/handouts/statistics.html
Note: These calculations are meant to provide information based on the study sample for comparison purposes, not to predict individual outcomes. The significance of these calculations depending on other important questions as described below:
Survival curves - the basics http://cancerguide.org/scurve_basic.html
"You will often find survival curves inhabiting technical papers in the medical literature, and some understanding of these curves is essential to understanding the technical literature."
Statistics (a primer):
The purpose of statistical analysis is to tell us how likely the finding in the experiment predicts outcomes in the real world. Was it fully or partially due to chance? What is the level of confidence?
Important questions to ask:
|
|
Is the question being asked relevant?
|
|
|
Do the data come from reliable sources?
|
|
|
Margin of error/confidence interval—when is a change really a change?
|
|
|
Are all data reported, or just the best/worst?
|
|
|
Are the data presented in context?
|
|
|
Have the data been interpreted correctly?
|
|
|
Does the author confuse correlation with causation?
Source: Statistics Handout http://www.unc.edu/depts/wcweb/handouts/statistics.html
|
Resources:
.gif) |
Statistics – CancerGuide: The Median ISN'T the Message
|
.gif) |
Statistics 101 - CancerGuide: Survival Curves
|
About statistical significance:
In order to draw better conclusions about data we need to know just a little about measures of statistical significance, which I think of as a level of certainty that an outcome was not due to chance.
So, hypothetically, if you gave two groups identical placebo therapies there would be a difference in the outcome - even if those two groups were quite large. That is, by chance one or the other group will do better given identical drugs because by chance they will have higher or lower risk disease, or capacity to heal, and so on. . So it's very common to see what looks to be a sizable difference in a study outcome be described as "no significant difference."
"Statistical conclusions, about responses to treatment in a small group of patients for example, are not absolute. Everything is possible, but some things are very possible, some are less possible and others are very unlikely -- but still possible to occur.
We draw conclusions with a certain amount of confidence, conventionally 95% or 99%,
but there is still some chance of an error (5% or lower)." Source: stanford.edu
Margin of Error - Confidence
We might just look for two measures of statistical significance in scientific reports to quickly estimate the strength of the finding: p-value and confidence interval.
If the p-value is .05 or less, the findings are considered statistically significant - not due to chance.
The confidence interval (CI) shows the level of confidence that the study outcome predicts the result in a larger population, expressed as a range. The wider the range, the less confidence we have that the results of the study predicts outcomes in the real world.
Measures of statistical significance
|
Value or range that indicates statistical significance
|
threshold probability value that tells you if outcome is due to chance
|
.05 or less
.01 is very good
.05 is on threshold (borderline)
.08 is not statistically significant
|
95% confidence interval (were the study repeated multiple times, it would contain the true effect 95% of the time) - a range of expected results.
|
71% (95% CI: 42-92%)
83% (95% CI: 63-95%)
94% (95% CI: 63-97%)
In the last example, we might say that we are 95% confident that the response rate is between 63 and 97%.
The wider the confidence interval the lower the confidence.
|
|
P-value or Probability value: A value that results from a calculation that tells you how likely or unlikely the finding (of a difference in treatment response as an example) was due to chance.
Common language for low p-value: Statistically significant - means unlikely due to chance.
Caveats about importance of P-value:
|
|
Threshold (cap) is arbitrary, therefore, the closer the p-value is to the threshold (.05), the less statistically significant.
|
|
|
Statistical significance does not necessarily = clinical importance.
|
|
|
Chance is rarely the most pressing issue. Biggest threat is systemic error (bias) Therefore more qualitative questions include: Are these the right patients? Are these the right outcomes? Are there measurement biases? Are observed associations confounded by other factors?
|
|
|
P values provide no information on the results' precision - that is, the degree to which they would vary if measured multiple times. Consequently, journals are increasingly emphasizing a second approach: reporting a range of plausible results, better known as the 95% confidence interval (CI). |
Factors that influence P-values:
|
|
Magnitude of the main effect: a larger difference will have a lower p-value·
|
|
|
Number of observations: a difference noted in a study of 500 patients will have a lower p-value than the same differences observed in a 25 pt group.
|
|
|
Spread of the data (standard deviation): if the observed differences in response are unified and less spread out, the p-value will be lower (more statistically significant)
Adapted from American College of Physicians-American Society of Internal Medicine |
|
|
95% Confidence Interval (CI):
"The interval computed from the sample data which, were the study repeated multiple times, would contain the true effect 95% of the time." " Where confidence intervals are wide, they indicate less precise estimates of effect." - med.ualberta.ca
Translation:
Studies on a limited number of patients can only estimate real world results; and if you did the same study 10 times (on different participants with same inclusion criteria), you would get different outcome each time.
So CI is a shorthand way to state this.
Example: in one study:
"Median duration of response was 21 months (95% CI, 18 to 24 months)."
The 95% part is to show, again, that the median outcome in any single trial cannot with 100% certainty predict outcomes for the entire population - in this case, all people with relapsed indolent lymphomas or MCL using this drug.
You can also think of the CI interval as a margin of error ... 21 (18 to 24 ) as done in election exit polls.
The narrower the CI interval, the more confidence there is in the finding. If the 95% CI was very wide (2 to 100) that would show very low confidence.
This ties into n (the number of patients in the study). In a ten patient study, the CI would be very wide - probably not even worth calculating - just as only 4 flips of a coin (all Heads) would not show the true odds of coin-flip outcomes.
The CI will widen (lower confidence) when the study population is small, and it includes a mix of lymphoma types.
How do you calculate the CI?
|
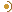
|
Use calculator: http://faculty.vassar.edu/lowry/prop2_ind.html
|
|
Also see:
|
|
Difference between p-value and confidence interval: musc.edu/
|
Three Measures of Association
(adapted from ASSOCIATIONS & CAUSATIONS http://www.sunmed.org/caus.html )
risk difference | risk ratio | odds ratio
Risk Difference (excess risk):
The difference in the incidence among those who are exposed and those who are unexposed.
EXAMPLE:
If the incidence of lung cancer among smokers is 10 per 1000 and incidence among non-smokers is 1 per 1000, then the risk difference is 10 per 1000, minus 1 per 1000 = 9 per 1000.
Risk Ratio (Relative Risk or RR):
The ratio of incidence among exposed and unexposed.
EXAMPLE: using the same smoking example above, this will be 10 per 1000 (smokers), divided by 1 per 1000 (non-smokers) = 10/1 or 10. An Relative Risk of 10 means that smokers have a 10 times higher risk of developing lung cancer compared to non-smokers.
A risk ratio is an extremely powerful measure of association. The greater the RR the more strength you have for the observed association (in other words, an RR of 10 implies a much stronger association between smoking and lung cancer compared to an RR of 2).
An RR of 1 implies no association between two variables. In practice, it's difficult to estimate the RR because true incidence figures are obtained only from studies which have a longitudinal component (cohort study) and such studies are difficult to do.
Hazard Ratio is a kind of relative risk
The hazard ratio is the effect of an explanatory variable on the hazard or risk of an event. (Wikipedia.org) ... such as the effect of a dietary practice (high red meat consumption) on mortality (the event) ... compared to those who have less of it.
If the Hazard Ratio (HR) is 1.00 there is no difference in the incidence of the event when the two patient groups are compared - one with the explanatory variable, the other without.
EXAMPLE: read meat consumption and mortality
(women): HR, 1.36 ... confidence range: [95% CI, 1.30-1.43]
(men): (HR, 1.31 ... confidence range: [95% CI, 1.27-1.35],
(modest increased risk of mortality from high red meet consumption)
EXAMPLE: Statins use during treatment in follicular lymphoma patients was also associated with better event-free survival (the measured event), though this difference was not statistically significant:
(HR = 0.67, ... confidence range: 95% CI: 0.39-1.16, p=0.15).
(NOTE: The Hazard Ratio (HR) above is less than 1, but the wide Confidence Interval (CI) and the fact that the higher range was above 1 indicates that this difference between the two patient categories could be from random variation - not statistically significant.)
Reference point: The Hazard Ratio for smoking (variable) and lung cancer (event) is
about 10 (range 2.35 to 19.33, depending on race)
Adapted from: http://www.dhr.dk/Glossary.htm
Odds Ratio or OR (Relative Odds):
The odds (not risk) of occurrence of an event or disease compared between two groups (exposed and unexposed).
An OR is usually computed in a case control study where it is not possible to get the true risk (incidence). Risk and odds tend to very similar when the disease occurrence is rare'.
EXAMPLE: If a group finds that lymphatic tissue from patients with NHL are 5 times more likely than controls (normal tissue) to have a certain virus, that would be expressed as
OR = 5. An OR of 1 would mean no difference between the two groups.
|
Absolute risk / Life time risk
The risk of developing a disease over a period of time. We all have absolute risks of developing various diseases such as heart disease, cancer, stroke, etc. The same absolute risk can be expressed in different ways. For example, you have a 1 in 50 risk of developing a lymphoma in your life. This can be expressed as a 2% risk, or a 0.02 risk.
Types of Clinical Data (most reliable first)
Randomized controlled clinical trials: (Provides strongest evidence of clinical benefit)
Participants are assigned randomly (by chance instead of by investigator selectioni) to separate groups (arms) for the comparison of different treatments -- usually a standard and an investigational treatment. Patient informed consent is required. Neither the investigators nor the patient choose the group in which participants will be placed.
Using chance to assign people to treatment arms helps to avoid selection bias -- putting pts in better health in the investigational arm, for example. It also helps to ensure that the groups will be similar and that the treatments they receive can be compared objectively.
Randomized trials can be "double-blinded" or "non-blinded." In double-blind studies, neither the investigator nor the participants are informed of which arm the participants have been assigned to. This also reduces bias and improves confidence in the findings.
NOTE: Systematic reviews that evaluate the outcomes in many trials, including randomized trials, may be the best source of evidence to guide clinical practice.
Nonrandomized controlled clinical trials
Participants are assigned to a treatment group based on criteria determined by the investigators, such as prognostic indicators, and disease type. This study design makes it possible for investigator bias to influence the findings, and therefore there is less confidence that the group receiving the treatment under study and the control group are comparable.
Case series (observational studies):
Case series are studies (usually retrospective) that describe outcomes, such as responses, time to progression, etc.) from patients who received the treatment under investigation.
These provide weaker evidence than do experimental studies because of the potential for biases such as, but not limited to, who is observed and what outcomes the observer is looking for, unknown association between factors and outcomes -- such as not accounting for other reasons that could explain the observed result.
The value of these types of studies (e.g., case series, ecologic, case-control, cohort) is that they provide preliminary evidence that can be used as the basis for hypotheses testing in stronger experimental studies, such as randomized controlled trials. Consider the recent HRT report finding that using estrogens increases the risk of heart disease and cancers. The hypothesis that it might reduce these risks was based on observations that were proven to be incorrect.
About press releases, and the reports you don't see
Protocols, ethical principles, and a desire to maintain credibility are beneficial forces that encourage responsible public reporting of drug development research and clinical trial outcomes.
But consider that an easy way to put a positive spin on a company's drug development project is to selectively report on favorable outcomes, and to keep less than stellar results from being released at all.
Ask: How is response to treatment being defined? How were the patients selected? How many patients were tested? What was the control? Has the finding been replicated by an independent group? Have all the study outcomes been reported? Is this an interim report, or a report on all - predetermined number of participants?
The Problems with Testimonials PDF version
"For many centuries doctors used leeches and lancets to relieve patients of their blood. They KNEW bloodletting worked. EVERYBODY said it did. When you had a fever and the doctor bled you, you got better. EVERYONE knew of a friend or relative who had been at death’s door until bloodletting cured him. Doctors could recount thousands of successful cases."
See also: When Laypersons Give Medical Advice
|
|
You can't tell in any individual case what would have happened if nothing was done, or something else
- particularly for a type of lymphoma that is known to wax and wane - that has a variable clinical course.
Further, cancers are heterogeneous - the genetic changes vary from person to person within the same type of cancer.
|
|
|
Such accounts can't inform about the number of persons who have used the intervention and did not benefit or were harmed.
There is no denominator - the number of patients studied.
The denominator tells us if the result are likely to occur in 1 of 5, or rarely - in 1 of 30,000.
Testimonials cannot provide even an estimate of a rate of effect in others,
or if the effect that is measured was even caused by the intervention.
In clinical science a pre-specified study size is required to provide a rate of an event or treatment effect.
A control group is often needed to establish causality - that the treatment (or part of the treatment) caused the outcome.
This is the reason that expensive and large controlled studies are often needed before a drug can be approved for the treatment of a disease.
|
|
|
People who die cannot testify
Patients who have tried and failed an alternative strategy cannot be accounted for.
Only the "successful" outcomes are reported, which may be 1 in many thousands.
Compare with peer-review clinical trial where the number of patients receiving the treatment
are known up front (prospectively), and the positive and negative outcomes are measured uniformly - and reviewed independently.
|
|
|
The authenticity of the report?
We cannot know if the person reporting the benefit really has the medical condition,
or if he or she is reporting the outcome accurately?
With testimonials there is no follow up, or independent review of the outcome over time.
Did the person relapse shortly after the testimonial?
|
|
|
The biases of the individual reporting the case?
Does the individual have a financial conflict of interest or strong belief?
Do they sell the product or charge a fee for dispensing the information?
Is the testimonial a way of validating their personal decision process and theories?
|
|
|
The specifics of the case, such as the natural history of the disease?
Even for cancers with a very poor prognosis there are case reports in the literature of spontaneous remissions, independent of any intervention.
Some types of cancer behave indolently -- and do not progress to a point requiring treatment.
People sometimes win the lottery , but this does not make playing the lottery a good bet - particularly when betting your life.
|
|

|
How the outcomes were measured, when, and by whom?
Was the reported success objectively measured and validated by independent physicians?
Is it a patient reported outcome?
Was it that the patient felt better?
What tests were used to measure it? What happened later?
... and did the intervention lead to a lasting and meaningful clinical benefit?
Is the condition self-limiting - does it sometime self-correct with time?
|
|
|
What other medical treatments were given shortly before or after?
A CT scan will often show lesions after standard treatment that are necrotic scar tissue. Credit might be given to an alternative practice used AFTER this treatment, when it was merely the resolution of a scar tissue over time, a normal bodily process.
Was the tumor removed by surgery prior to the alternative practice?
|
|
|
The accuracy of the diagnosis?
Was it a false diagnosis of a cancer, or a cancer of a type with an indolent course?
|
For all of these reasons it's prudent to regard testimonials with suspicion - particularly if the report is implausible, scientifically. Scientists get cancer too, as do their children. Do scientists think the approach is plausible?
Similarly, case reports have many of the above limitations - cannot establish causality, and can't be the basis for predicting outcomes in others. For example, if one patient receives regular treatment followed by a study drug, it's not possible to be certain that the second part of the treatment improved the outcome.
Related Topics:
|
|
"Anecdotal evidence. An oxymoron?
Or a valid approach to understanding data? scienceb asedmedicine. org
|
|
|
|
In-vivo or in-vitro? - in-vitro means in test tube or cell culture; in-vivo means in the body.
We frequently read or hear about the anti-cancer properties of this or that supplement based on scientific research findings. Here are some questions to ask of this kind of information:
|
|
Was the response detected in a test tube (in-vitro/cell culture)?
The human body is infinitely more complex than a test tube.
The tumor cells change when removed from the body; oftentimes they will die spontaneously.
Nevertheless, indications of activity in a test tube often become the basis for product claims about natural supplements. Be aware that this can only be a starting point for additional experiments. Using such data as the basis of medical claims is irresponsible, and bias should be suspected. Furthermore, you might ask if the dose used to produce the in-vitro effect possible to achieve in the body, or if it can be achieved safely?
|
|
|
|
Animal studies?
Is the claim for the promise of a drug or supplement based solely on animal studies? While animals are useful for preclinical testing of new drugs, there are many differences between animals and humans; and drugs that show promise in tumors implanted in animals are not always effective in cancers originating in humans, or can be given safely to humans.
See also A Mouse is not a Man (or Woman) |
|
Weighing Sources of Medical Evidence
Weight
Evidence for Clinical Benefit?
|
Description with notes
|
|
Best
Random selection prevents patient-selection bias -- "cherry picking" lower-risk participants in the study arm.
Provides the most objective basis for understanding risks and benefits.
|
Phase III randomized, blinded, multi-center studies
Best if studies had large numbers of participants, and the results are confirmed by other studies completed by independent groups.
The data from phase III studies are subject to peer review and sometimes to impartial independent 3rd-party review, such as FDA.
Systematic Review is a study of studies, including randomized types. A systematic review may provide strongest evidence to guide clinical practice.
Look for the reputation of the journal - it is best if published in highly respected, peer-review journal.
Best results will show low p-values and narrow confidence intervals.
P-values < .05, or lower are considered statistically significant (not due to chance), but this does not speak to potential weaknesses in the endpoint.
The analysis should include all of the participants in the study - the intent-to-treat population, not a subset.
Randomized studies do not show best use, necessarily, but provides the best information about risks and benefits for a specific condition and setting, relative to the control - typically the standard of care.
|
|
Low to Moderate
Subject to patient selection-bias
|
Phase II studies - typically small single-arm studies that look for indications of clinical activity and safety, and sometimes explore dose or dose schedule
Determine if phase III testing is worth effort and expense, and importantly, if potential benefits offset risks to future study participants.
Phase II studies are often not conclusive. (Watch for sponsor hype in press releases.)
If the safety and signals of activity are good, data from phase II studies might provide the rationale for phase III testing.
|
|
Low
dose-finding, safety study
|
Phase I studies - earliest clinical phase: dose-finding studies in human subjects.
This type of study cautiously seeks bioavailability and safety information with close supervision of the participants. For example, helps to determine if the drug goes to target cells, or organs of concern.
Most drugs fail at this phase, but even the great ones start here. Typically participants have tried and failed other options.
|
|
Low
Hypothesis forming
|
Case studies - anecdotal reports made by physicians, usually for off-label use of an approved drug, for which there is existing safety information.
Hypothesis forming. Rationale for use is often mechanism-based. Note that the rationale for Hormone Replacement Therapy was supported by observation and case reports, and proven incorrect in a controlled study.
|
Lower
Still
Hypothesis forming
|
Animal studies provide (imperfect) models for what might happens in humans.
These next-step experiments provide clues about toxicity and bioavailability of agents shown to have activity in cell culture experiments.
Tumors are often transplanted into animals - setting up an artificial host/tumor environment. Animal studies can't account for important differences in biology, metabolism, tumor/host interactions in humans.
|
|
Lowest
Hypothesis forming
|
cell culture (in-vitro) These are first-step experiments to show the activity of compounds on cultured cancer cell lines, often of limited types and strains ... cells that that have been removed from the host environment ... And like a fish out of water, these cells do not behave like cancer cells in the body. Consider that even malignant cells, resistant to cell death in the body, will die spontaneously when removed from the body and put into cell cultures.
Further, according to some sources, approximately 1 in 5,000 agents showing activity in cell culture assays (such as a change in proliferation rate) will become useful therapeutic agents.
Such experiments lack information on bioavailability, toxicity or activity in the body at clinically relevant doses.
Thus the results of in-vitro experiments are hypothesis forming -- where research starts; not what conclusions can be based on.
Unfortunately, the limitations of in-vitro experiments are not always explained in ads for herbal products promoted as having anti-cancer activity in cell culture experiments.
See also
Preclinical development of molecular-targeted agents for cancer nature.com
|
| Cause for suspicion |
testimonial - Anecdotal reports made by individuals about improvements in health associated with an intervention.
Testimonials are sometimes found on commercial sites as a marketing strategy. Reliance on testimonials is a red flag that controlled studies have not been done, else the study, and not the story, would be the basis for the promotion.
Limitations of testimonials - they cannot inform about (1) who is reporting the result; if they have biases or conflict of interest - or if it is truthful account; (2) the case details, such as prior or subsequent treatments, or how the reported benefits were measured, or how long the reported benefits lasted. (3) The background, such as the natural history of the disease. (4) There is no way to know if negative reports are excluded - those who die cannot provide a testimonial.
|
| NOTES: |
Not every scientific paper that is published is of high quality.
Concentrate on the study methods (such as the number of participants and how they were selected, how long the follow up), not the conclusions of the study authors
Have the outcomes been reproduced by another research group?
An active drug stops or interrupt a disease process, such as cell division in cancer, but an active drug is not necessarily an effective drug, because the side effects of the drug might offset the positive effects.
|
References and Related Articles
-
Background articles on Evaluating Medical Information - PAL
-
The limits of evidence-based medicine. Respir Care. 2001 Dec;46(12):1435-40; discussion 1440-1. Review. PMID: 11728302
-
The Product Pipeline and Clinical Trials: Bringing a Drug to Market - biology.iupui.edu
September 6 and 8, 2005
-
The Dirt on Coming Clean: Perverse Effects of Disclosing Conflicts of Interest
cbdr.cmu.edu .pdf
|
|
|