Related Topics
|
|
|
|
| AANS |
American Association of Neurological Surgeons |
| ADCC |
Antibody-Dependent Cell-mediated Cytotoxicity. Immune response triggered by presence of antibody, Abs, coating the target cell, (such as Rituxan). |
| Adenocarcinoma |
Tumor derived from glandular structures…present within the mucosal linings…urinary tract… |
| Adjuvant |
Auxilliary, added to improve action of that to which it is added. (Neo-adjuvant is an intervention that is given before another.) |
| Adrenal cortex |
Outer portion of adrenal glands, secrete steroids that inhibit inflammation in allergic responses. |
| Alemtuzumab |
Humanized monoclonal antibody, anti-CD52. Used against CLL, et. al. |
| Allele |
Any one of a series of two or more different genes that occupy the same position(locus) on a chromosome. |
| Allogeneic |
Referring to genetically different cell lines, in one individual, capable of producing different antigens. |
| AML |
Acute Myelogenous Leukemia or Acute Myeloid Leukemia. |
| Amyloid |
Glycoprotein deposited extracellularly in tissues in amyloidosis. |
| Amyloidosis |
Any of a variety of diseases that deposit amyloid material in tissues. Primary has no obvious predisposing condition. Secondary is associated with another chronic disease such as TB. |
| Anabolic |
Of, or related to, the synthetic phase of metabolism. |
| Anabolism |
Synthesis of more complex substances from simpler ones. |
| Analogue |
Chemical compound with a structure similar to that of another but differing from it in respect to a certain component; it may have a similar or opposite action metabolically. |
| Aneuploidy |
One or a few chromosomes above or below the normal chromosome number; e. g., three number 21 chromosomes, or trisomy 21 (characteristic of Down Syndrome) is a form of aneuploidy. |
| Anthracycline |
A type of antibiotic that comes from the fungus Streptococcus peucetius. Some are daunorubicin, doxorubicin and epirubicin. |
| Antibody |
Immunoglobulin molecule evoked by an antigen (immunogen). It interacts with the antigen, that induced its synthesis, in some demonstrable way. |
| Antigen |
Any substance, toxin or enzyme, that stimulates the production of antibodies. |
| Antigenicity |
Ability of a substance to trigger an immune response to a particular organism. |
| Antineoplastic |
Inhibiting or preventing development of neoplasm, checking maturation and proliferation of malignant cells. |
| Apheresis |
Peripheral blood stem cell harvesting. |
| Apical |
Relating to apex or tip; situated near the apex of a structure; opposite of basal. |
| Apoptosis |
Ap-o-TOE-sis. A normal series of events in a cell that leads to its death. |
| Ascite |
Effusion and accumulation of serous fluid in abdominal cavity; AKA abddominal or peritoneal dropsy, hydroperitonea, and hydrops abdominis. |
| Asthenia |
Weakness or debility. Syn: Adynamia |
| Ataxia |
Failure of muscular coordination; irregularity of muscular action. |
| Atopic, atopy |
Clinical hypersensativity state or allergy with a hereditary predisposition. The tendency is inherited, but the specific clinical form (hay fever, asthma,…) is not. |
| Autologous |
Produced from the subjects own tissues. |
| Autophagy |
NCI: "A normal process in which a cell destroys proteins and other substances in its cytoplasm (the fluid inside the cell membrane but outside the nucleus), which may lead to cell death. Autophagy may prevent normal cells from developing into cancer cells, but it may also protect cancer cells by destroying anticancer drugs or substances taken up by them." |
| BEAM |
BCNU (carmustine), cytarabine, etoposide, melphalan. |
| BID |
Twice a day (bis in die) |
| Biliary |
Relating to bile or the biliary tract. |
| Biotherapy |
Biological therapy. Treatment by injection of substances that produce some biological reaction; antitoxins, vaccines,… |
| Cachexia |
ka kek' see a - Weight loss. |
| Carcinoma |
Cancer that begins in the skin or tissues that line or cover internal organs. |
| Casuistry |
1. Application of general rules and principles to questions of ethics or morals in order to resolve them. 2. Use of subtle, sophisticated, and sometimes deceptive reasoning, esp. on moral issues, in order to justify something or mislead somebody. |
| CBCL |
Cutaneous B-Cell Lymphoma |
| CCIR |
Center for Cancer Immunology Research |
| Chimeric |
Composed of parts of different origin and are seemingly incompatible (e. g.,mouse and human?) |
| CHOP |
Cytoxan, Hydroxyrubicin (Adriamycin), Oncovin (Vincristine), Prednisone |
| Cisplatin |
Cis-isomer of a platinum compound that has antineoplastic action and may enhance tumor antigenicity. |
| CLL |
Chronic Lymphocytic Leukemia (Indolent) |
| Cloaca |
Klo-aa'-ka In embryology, the terminal end of the hindgut before division into rectum, bladder and genital primordia. |
| CML |
Chronic Myelogenous Leukemia |
| CNOP |
Cycolphosphamide, Mitoxantrone, Vincristine (Oncovin), Prednisone |
| CNS |
Central Nervous System |
| Cohort |
In epidemiology, a group of individuals who share a common characteristic, statistical factor. The term always indicates observation of the individuals over time. |
| CPOP |
Pixantrone, Cyclophosphamide, vincristine (Oncovin), and Prednisone. |
| CR |
Complete Response |
| CVP |
Chemo regimen of Cyclophosaphamide, Vincristine and Prednisone. |
| Cystectomy |
Surgical removal of the bladder. |
| Cytokine |
A generic term for hormonelike, nonantibody, low-molecular-weight proteins secreted by various cell types on contact with specific antigens. They act as intercellular mediators, as in the generation of an immune response. These are the "interleukins". |
| Cytology |
Study of cells, their origin, structure, function and pathology. |
| Cytolytic |
Having a destructive effect on cells. |
| Cytoma |
General term for a cell tumour such as a sarcoma. |
| Cytopenia |
Reduction of the number of cells circulating in the blood. |
| Cytophotometry |
Study of organic compounds within cells by measuring the light through selected stained areas of cytoplasm. |
| Differentiation |
Maturity of cancer cells, ie, degree to which they resemble normal cells. The more mature, ie, the closer the resemblance, the slower growing and the better the prognosis. The less the resemblance, the more uncontrollably they grow. |
| Diplopia |
Perception of two images of a single object. |
| Diuresis |
Increased production of urine. |
| DLBCL |
Diffuse Large B-Cell Lymphoma |
| DNA |
Deoxyribonucleic acid. Molecule of two long strands that form a double helix and on which all genetic information is encoded. |
| Dyscrasia |
Disease or pathologic condition. |
| Dyspnea |
Shortness of breath, a subjective difficulty or distress in breathing. |
| Dysuria |
Difficulty or pain in urination. |
| Electrophoresis |
Separation of ionic molecules (principally proteins) by the differential migration through a gel according to the size and ionic charge of the molecules in an electrical field. |
| Endocytosis |
Uptake of a material into a cell by the formation of a membrane bound vesicle. |
| Endogenous |
Originating or produced within the organism or one of its parts. |
| Endometrium |
The tissue lining of the uterus. |
| Epistaxis |
Nosebleed. |
| Epithelium |
Covering of internal and external surfaces of the body. |
| Epitope |
The simplest form of an antigenic determinant, on a complex antigenic molecule, which can combine with antibody or T-cell receptor. |
| Erythema |
Redness due to capillary dilation. |
| etiology |
The study of factors that cause disease and their method of introduction to the host; causes or origin of a disease or disorder. |
| Extramedullary |
(Coupled with "haematopoiesis") The formation and development of blood cells outside the bone marrow, as in the spleen, liver or lymph nodes. |
| Extramedullary plasmacytoma |
Monoclonal plasma cell infiltrate of tissues other than bone. |
| Febrile |
Fee-brul, Pertaining to fever. |
| FISH |
Fluorescence in situ hybridization, a molecular technique used in chromosome studies. The process vividly paints chromosomes, or portions of chromosomes, with fluorescent molecules. |
| Fistula |
Abnormal passage or connection. |
| FL |
Follicular lymphoma, the most common form of NHL. |
| FLIPI |
Follicular Lymphoma International Prognostic Index. Main purpose appears to be to characterize participants in clinical trials. May, sometimes, be used in selecting treatments and timing of treatments. |
| Flow Cytometry |
Immunophenotyping method using fluorescently labeled antibodies on specimen cells in fluid, forced through an orifice, such that individual cells pass through a laser beam one at a time. The cytometer counts the cells that fluoresce. |
| FND |
Chemo regimen of Fludarabine, Mitoxantrone (Novantrone) and dexamethasone. |
| Fulguration |
Destroying tissue using an electric current. |
| Gammopathy |
A condition of the immune system characterized by an abnormal increase in the levels of immunoglobulins in the blood. (See attachment) |
| GBM |
Glioblastoma Multiforme (The most dangerous type of brain tumor) |
| Genotype |
The genetic constitution of an organism or cell, as distinct from its expressed features or phenotype. |
| HAMA |
Human Anti Mouse Antibody |
| Hapten |
A molecule, incapable alone, of causing production of antibodies, but can combine with a larger antigenic molecule, a carrier. A heptan-carrier complex can stimulate production of antibodies, some of which combine with the hapten portion of the complex. |
| HDAC inhibitor |
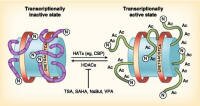 The class of drugs known as histone deacetylases (HDACs) appear to be active against cancer cells by loosening the grip of histones within a cell - restarting tumor suppressor genes (built in protections against cancer within the cells) helping to cause the tumor cells to die or to stop growing. The class of drugs known as histone deacetylases (HDACs) appear to be active against cancer cells by loosening the grip of histones within a cell - restarting tumor suppressor genes (built in protections against cancer within the cells) helping to cause the tumor cells to die or to stop growing. |
| Helminthic |
Pertaining to, or caused by, parasitic worms. |
| Hematocrit |
Relative volume of blood occupied by erythrocytes, i.e., red blood cells that carry oxygen to all parts of the body. An avg figure for humans is 45 ml per cent, i.e., a packed red cell volume of 45 ml in 100 ml of blood. |
| Hematopoietic |
Pertaining to the formation of blood cells. |
| Hematuria |
Presence of blood, or red blood cells, in the urine. |
| Hepatorenal |
hep a to ren' al Relating to the liver and kidney. Syn: hepatonephric |
| Hepatosplenomegaly |
Abnormal enlargement of both liver and spleen. |
| Hepatoxicity |
Toxic to liver cells. |
| Hilum (Hepatic) |
The part of an organ where the nerves and vessels enter and leave. |
| Histocompatibility |
Ability to be accepted and remain functional. |
| Histology |
Study of cells and tissues at microscopic level. |
| Histology |
The microscopic appearance of biopsy cells. |
| HLA |
Human Leukocyte Antigen. |
| Homeostasis |
Tendency of a physiological system to remain more or less stable. |
| HPV |
Human Papillomavirus |
| Hypercal'cemia |
Excessive amount of calcium in the blood. |
| Hyperemic |
Increased amount of blood flow in a part or organ. |
| Hyperuricemia |
Enhanced blood concentrations of uric acid. |
| Idiopathic |
Cause unknown |
| Idiotope |
Single antigenic determinant of an idiotype. |
| Idiotype |
Collection of idiotopes that confers on Ig molecule an antigenic individuality. Frequently a unique attribute of a given antibody. A unique cell marker. |
| IFN |
Interferon |
| IGIV |
Immune Globulin Intravenous. |
| Immunogenic |
Evoking an immune response. Producing immunity. |
| Immunoglobulin |
A protein, produced by plasma cells, that acts as an antibody fighting infections, allergens, tumors,… |
| Immunopathogenesis |
Process whereby an immune response changes the development of disease. |
| Immunophenotype |
Specific repertoire of proteins displayed on cell surface. |
| Immunoscintigraphy |
Scintigraphy of antibodies labeled with radioactive substances. |
| Immunotherapy |
Treatment to stimulate immune system. A.K.A. biological therapy, biotherapy, or biological response modifier (BRM) therapy. |
| In vitro |
In a glass, observable in a test tube. |
| In vivo |
Within the living body. |
| Inflammatory mediators Molecules released by immune cells when harmful agents invade. |
| Intrathecal |
Into the spinal fluid; into a sheath |
| IPI |
International Prognostic Index. Predicts risk of lymphoma recurrence and overall survival. Factors: age, stage, general health, number of extranodal sites and LDH level. |
| Karyotype |
Characterization of chromosomal complement of an individual or species, including number, form and size of chromosomes. |
| KLH |
A substance taken from a marine organism that may be linked to a specific antigen to boost the immune response to that antigen. KLH is being studied as a way to increase the immune response to cancer vaccines. It is a type of immune modulator. Also called keyhole limpet hemocyanin.
|
| Lamina Propria |
A thin vascular layer of connective tissue beneath the epithelium of an organ. |
| Ligand (NCI definition) |
"A molecule that binds to another molecule, used especially to refer to a small molecule that binds specifically to a larger molecule, e.g., an antigen binding to an antibody, a hormone or neurotransmitter binding to a receptor, or a substrate or allosteric effector binding to an enzyme. Ligands are also molecules that donate or accept a pair of electrons to form a coordinate covalent bond with the central metal atom of a coordination complex." |
| LDH |
Lactase dehydrogenase; enzyme in blood disease indicator. |
| Lesion |
Any pathological or traumatic discontinuity of tissue or loss of function of a part. |
| Leukopenia |
The antithesis of leukocytosis; any situation in which the total number of leukocytes in the circulating blood is less than normal, the lower limit of which is generally regarded as 4000 to 5000/mm^3. Syn: leukocytopenia. |
| LLMPP |
Lymphoma/Leukemia Molecular Profiling Project. |
| LPL |
Lymphoplasmacytic lymphoma. |
| Lymphadenopathy |
Disease or swelling of the lymph nodes. |
| Lymphocyte |
White cells, B (differentiate in bone marrow) and T (differentiate in Thymus), for immune responses in the bodily humors (fluids) and cells, respectively. |
| Lymphokine |
Lim' fe kine, Substance released by T cells that have been activated by enzymes. Activate macrophages. |
| Lymphoma |
Neoplasm of lymph tissue, usually malignant. |
| Lymphopenia |
A reduction, relative or absolute, in the number of lymphocytes in the circulating blood. Syn: lymphocytic leukopenia, lymphocytopenia. |
| Lysis |
Rupture of cell membranes and loss of cytoplasm. |
| Lytic |
Pertaining to cell destruction (lysis). |
| Macrophage |
A type of white cell that surrounds and kills microorganisms, removes dead cells, and stimulates the action of other immune cells. |
| Malignant |
Tending to invade and destroy nearby tissue and to spread to other parts of the body. Tending to become progressively worse and to result in death. |
| MCL |
Mantle cell lymphoma. |
| MDS |
Myelodysplastic syndromes. |
| Mediate |
To cause a change as in stimulation by a hormone; accomplish by the aid of an intervening medium. |
| Medulla |
The inner portion of an organ. |
| Medullary |
Pertaining to the marrow or any medulla resembling the marrow. |
| Melanoma |
A form of skin cancer that arises in melanocytes, the cells that produce pigment. Usually begins in a mole. |
| Mele'na (ee') |
Passage of dark colored, tarry stools, due to blood altered by intestinal juices. |
| Mesothelioma |
Malignant tumour of the mesothelium, usually of lung, caused by exposure to asbestos fibres,… |
| Mesothelium |
Single squamous epithelium of mesodermal origin. It lines the peritoneal, pericardial and pleural cavities and the synovial space of the joints. |
| MGUS |
Monoclonal Gammopathy of Uncertain Significance. |
| MHC |
Major Histocompatibility Complex. The set of gene loci specifying major histocompatibility antigens, e.g., HLA in humans, DLA in dogs, H2 in mice, RLA in rabbits, RT1 in rats, SLA in pigs, etc. |
| Mitochondrion |
Mai-tE-kan-dri-En, Structures that occur in nearly all cells of plants and animals, and that process food for energy. |
| Mitosis |
Also karyokinesis. Cell division. |
| Moiety |
Moy'I tee; Any equal part; a half; also any part or portion. |
| Monoclonal |
Of a single clonal origin. |
| Monocytopenia |
Abnormal decrease in the proportion of monocytes in the blood. |
| Morbidity |
A diseased state. The frequency of the appearance of complications following a surgical procedure or other treatment. |
| Morphology |
The form or structure of a particular organism, organ or part. |
| Mucinous carcinoma |
A type of cancer that begins in cells that line certain internal organs and produce mucin. |
| Multiple Myeloma |
Uncontrolled growth of plasma cells, most common primary malignant neoplasm of bone. |
| Myalgia |
Muscular pain. Syn: Myodynia. |
| Myeloablative |
Severe myelosuppression, i.e., suppression of bone marrow activity. Reduces platelets, red cells and white cells. [Myel(o)] pertains to bone marrow or spinal cord or myelin (in this case, bone marrow). |
| Myeloma |
Cancer that arises in plasma cells. |
| Myelosuppression |
Bone marrow suppression, i.e., decrease in hematopoietic activity. |
| Myelotoxicity |
Destructive to bone marrow. |
| NCI |
National Cancer Institute |
| Neoplasia |
New growth, usually referring to abnormal new growth and thus a tumor. |
| Neoplasm |
New and abnormal growth of tissue which may be benign or cancerous. |
| Neoplastic |
Pertaining to or like a neoplasm with new and abnormal growth. Pertaining to neoplasia with the formation of a neoplasm. |
| Neurogenic |
1. Forming nervous tissue. 2. Originating in the nervous system or from a lesion in the nervous system. |
| Neutropenia |
Decrease in number of neutriphils in the blood. |
| NF |
Nuclear Factor. NF-kappaB is a protein complex, transcription factor, associated with cellular immune response and with cancer. |
| NIH |
National Institutes of Health |
| Nucleotide |
Basic structure of nucleic acid (RNA or DNA). |
| Oligonucleotide |
A short polymer of two to twenty nucleotides. |
| Oligosaccharide |
A saccharide of a small number of component sugars. |
| Oncogene |
A gene that causes the transformation of normal cells into cancerous tumor cells. |
| Oncogenic |
Causing the formation of tumors. |
| Paramagnetic |
1. Magnetic as opposed to diamagnetic, which means, repelled by the poles, positioning at right angles to magnetic lines of force rather than behaving like ordinary magnetic bodies such as iron. 2. Having a weak magnetic susceptibility. |
| Paraprotein |
Abnormal monoclonal immunoglobulin characteristic of, and produced by, malignant cells of the mature B-cell type, e.g., multiple myeloma. |
| Parenchyma |
The essential or functional elements of an organ. |
| Pathogenesis |
Source or development of a disease or disease process;cellular events and reactions that occur during a disease development. |
| Pathology |
Medical study of disease, esp. changes in tissues and organs that cause, or are caused by the disease. |
| Pathway |
In research papers we often see references to drugs that target PATHWAYS in cancer cells, which can be intimidating because of the cryptic names given to these unfamiliar functions within the cells, such as PI3K, or Akt, or, mTOR, or ALK
The exhaust, electrical and fuel systems of our cars might help to understand was is meant by a pathway in a cell.
The mechanic’s job is to diagnose the problem – usually by first identifying the system that is most likely to be causing the bad "behavior" of your car.
... Such as: is there a spark? If no spark is seen, the problem is most likely in the electrical system or "pathway."
The next step in the diagnosis is to find where the problem exists in the system.
For example, the fuel system has a storage tank, fuel lines, filters, pumps, vacuum hoses, and a carburetor - where air and fuel are mixed and then injected into the cylinder where the combustion occurs (where the spark meets the fuel) where one part of the system meets the other.
So in the jargon of cell biology, the fuel tank is “upstream of” (comes before) the fuel line, which is upstream of the carburetor, which comes before the cylinder where the combustion occurs, and so on.
Similarly, we might read in a cancer research paper:
“Upstream signaling inhibition enhances rapamycin [the drug] effect on growth of cancer cells” to mean: a narrowing or blockage in the fuel line (upstream of the carburetor) caused the engine to run slower or stop.
So while human cells are many times more complex than the familiar automobile engine, there are similarities that are sufficient to give us a feel for the biology of abnormal cells .. what the heck the researchers are talking about!
Why bother? You don’t have to be a mechanic to effectively drive a car, but it can help when you have a serious problem to have a feel for the subject – as in: does this mechanic's proposed remedy (for my car that is running too fast) seem plausible before you decide to let him fix it?
To when you read about a drug that targets the XYZ pathway, keep in mind that it's just a name (made up by somebody) for a system within a cell - which “drives” the bad behavior of the cell - such as rapid cell division and a refusal to shut down and die.
|
| PCR |
Polymerase chain reaction. A technique by which tiny amounts of DNA or RNA can be specifically identified. |
| Perivascular |
Situated around or near a vessel. |
| PET scan |
Positron Emission Tomography; images metabolic activity of body tissues. |
| Peyer's patches |
Areas of the intestinal wall which contain normal MALT. |
| Phagocyte |
A cell capable of phagocytosis. The main mammalian phagocytes are neutrophils and macrophages. |
| Phagocytic |
Pertaining to , or produced by, phagocytes. |
| Phagocytosis |
Killing and digesting of particulate material such as microorganisms. |
| Phenotype |
The total characteristics displayed by an organism under a particular set of environmental factors, regardless of the actual genotype of the organism. Results from the interaction between the genotype and the environment. |
| phoresis (suffix) |
Transmission. |
| Plasma cells |
White blood cells, produce antibodies. |
| Plasmacytoma |
Cancer of the plasma cells, may turn into multiple myeloma. |
| Plasmaphoresis |
Process of separating certain cells from plasma in the blood by machine; only the cells are returned to the patient. Can be used to remove excess antibodies from the blood. |
| Ploidy |
The number of sets of chromosomes within a cell or organism. |
| Pneumaturia |
Passage of gas in the urine, usually as the result of a fistula between the bladder and intestine. |
| poiesis |
A word termination meaning formation. |
| PR |
Partial Response |
| Progenitor` |
Parent or ancestor. |
| Protease |
PRO-te-az, Enzymes that degrade protein molecules, i.e., catalyze the hydrolytic breakdown into peptides or amino acids. |
| Proteolysis |
Cleavage of proteins by proteases. |
| Proteolytic |
Pertaining to, characterized by or promoting proteolysis. |
| Pruritus |
Itching |
| PTLD |
Post Transplant Lymphoproliferative Disease |
| Purine |
Colorless crystalline heterocyclic compound which is not found free in nature, but is variously substituted to produce a group of compounds known as purines or purine bases of which uric acid is a metabolic end product. The purine bases include adenine and quanine, which are constituents of nucleic acids, and hypoxanthine and xanthine. |
| QD |
Once a day (quoque die) |
| QID |
Four times daily |
| R-CVP |
Rituximab, Cyclophosphamide, Vincristine, Prednisone |
| Reticuloendothelial |
Relating to the widely diffused bodily system constituting all phagocytic cells except certain white blood cells. |
| Retroperitoneum |
Retroperitoneal space. Space between the perietal peritoneum and the muscles and bones of the posterior abdominal wall. Contains kidneys, suprarenal glands, ureters, duodenum, ascending and descending colon, pancreas, and the large vessels and nerves. |
| R-FCM |
Rituxan plus standard chemo of fludarabine, cyclophosphamide and mitoxantrone. |
| RNA |
Ribonucleic acid. A single strand molecule that conveys DNA information to ribosomes to instruct synthesis of a specific protein. Its sugar component of the nucleotides is ribose vs deoxyribose of DNA. |
| Sarcoma |
A form of cancer that arises in the supportive tissues such as bone, cartilage, fat or muscle. |
| Scintigraphy |
Diagnostic technique…two dimensional picture of bodily radiation source obtained by use of radioisotopes. From scintillation counter used to record radiation on the picture. |
| Senescence |
State of growing old. Decay by time. |
| Serology |
A blood test that detects the presence of antibodies to a particular antigen. Branch of science concerned with serum, esp. with specific immune or lytic serums; to measure either antigens or antibodies in serum. |
| SLL |
Small lymphocytic lymphoma. |
| Somatic |
Any cell except a germ line cell. |
| Splenomegaly |
Enlargement of the spleen. |
| Squamous |
Scaly or platelike. |
| Stasis |
Stoppage or cessation. |
| Stem cell |
Cell that gives rise to a lineage of cells. Most primitive cell found in bone marrow from what all various types of blood cells are derived. A cell that, upon division, produces dissimilar daughters, a replacement for the original and one that differentiates further. |
| Syngeneic |
Genetically identical, esp. w/ respect to antigens or immunological reactions. |
| Telomerase |
DNA enzyme that will elongate only oligonucleotides from the telomere. |
| Telomeres |
Tel' u mir, Either of sections of DNA occurring at the ends of the chromosome. |
| Thrombocyte |
Platelet. |
| Thrombocytopenia |
Decrease in number of platelets in the blood. |
| Thymocyte |
Lymphocyte found in the thymus; about 10% are mature T, and rest immature precursors in various stages of maturation. |
| TID |
Three times daily (ter in die) |
| TNF |
Tumor Necrosis Factor: Either of two (alpha or beta) lymphokines, produced primarily by cells of the immune system, capable of causing in vivo hemorrhagic necrosis of certain tumor cells, but not normal cells. |
| Transcription |
Synthesis of RNA by RNA polymerases using a DNA template. |
| Tumour |
Abnormal mass of tissue that results from excessive cell division that is uncontrolled and progressive. Also called "Neoplasm". |
| Urine Immunofixation |
Special lab technique used to identify specific proteins in the urine (or blood). Greatest application, identify monoclonal proteins produced by conditions like Waldenstrom's macroglobulinemia and multiple myeloma. |
| Urotheliotrophic |
(Not in dictionaries) Relating to a transitional wall of epithelium, in the bladder, and its nutrition. |
| Urticaria |
(er' ti kar' ea) An eruption of itching wheals (welts), usually of systemic origin. |
| Vascular |
Characterized by, or containing, vessels for carrying fluids, e.g., lymph or blood in animals or sap in plants. |
| Vasogenic |
Pertaining to blood vessels. |
| Vesical |
Relating to any bladder, usually the urinary bladder. |
IMMUNE SYSTEM TERMS
A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
active immunity is an acquired immunity in which the immune system recognizes an antigen as foreign and generates an attack on the invading pathogen or abnormal cell that expresses the antigen (a unique protein signature). The goal of cancer vaccines is to induce active immunity against unique proteins specific to the tumor cells. Here the immune system "learns" about the identity of part of the tumor and "remembers" this information in order to produce a sustained attack and long-term surveillance against the cancer cells.
agammaglobulinemia - a deficiency or lack of immunoglobulins, or antibody.
allergen - a substance that causes an inappropriate reaction by the immune system to normally harmless substances.
anaphylactic shock - a life threatening allergic reaction causing swelling, difficulty breathing, and a drop in blood pressure.
anergy - describes an unresponsive state of immune cells to antigen stimulation.
adaptive Immunity (specific immunity) is a response to a specific immune stimulus (antigen) that involves cells of the immune system and frequently leads to a state of immune memory. The adaptive immune system marshals antibodies and T cells that are highly specific for a particular pathogen (or antigen). Once created, the antibodies and T cells can eliminate the pathogen if it appears even years later - so-called immune surveillance.
antibody (Ab) - a protein molecule (also called an immunoglobulin) secreted by B cells in response to an antigen (Ag). When an antibody attaches to an antigen, it destroys the antigen.
Antibody-dependent Cell-mediated Cytotoxicity (ADCC) - An immune response triggered by the presence of antibody (Abs) coating the target cell (such as Rituxan). Upon binding its antigen, the Antibody's Fc region is exposed and will bind its receptor on the NK cell (or other effector cells) to form a bridge. Once the bridge is formed, a poorly understood lytic (killing) signal is delivered to the target cell by the effector cell, resulting in its demise. - (adapted from the Merck Manual) Picture-it
antigen - the portion of a foreign substance or germ that can cause the immune system to become active against it. Also from Merck Manual: "Substances that stimulate an immune response in the body are called antigens. Antigens may be contained within or on bacteria, viruses, other microorganisms, or cancer cells. Antigens may also exist on their own—for example, as pollen or food molecules. A normal immune response consists of recognizing a foreign antigen, mobilizing forces to defend against it, and attacking it."
antigen presenting cell (APC) - immune cells - such as b-cells, macrophages, and dendritic cells - that recognize foreign antigens, and present it to T-cells to initiate an immune response.
antigen receptors - molecules on the surface of b- and t-cells that allow the cells to engage a specific antigen in the body in order to mount an immune response that is specific to the foreign molecule it binds to.
antibiotics - Medicines used to treat some bacterial diseases.
apoptosis is a natural mechanism by which cells "commit suicide" when they have outlived their purpose, become defective, or have aged. Apoptosis prevents cells from accumulating and forming tumors. Understanding of the control of apoptosis in normal and malignant cells will help to improve the diagnosis and treatment of malignancies. The goal of many treatments, including chemotherapies is to induce malignant cells to undergo apoptosis. Picture it
Analogy: Chances are you've seen a movie with apoptosis as part of the plot ... in almost any James Bond film.
A fortress containing classified information is rigged for destruction by the owners if the security of the building is compromised. The process requiring a series of commands, which are relayed from one authorized person to another. This to prevent a programmed self-destruction by a careless mistake or a rouge individual.
The fail safe system is carried out from within by specialists, and regulated by others. The trigger is not pulled until all the criteria is met: the security threat is real and it can't be corrected; the command has been given by authorized individuals and verified by others, and the actions carried out by specialized personnel.
The security breach starts a chain of events (a cascade); each player communicating to the other until the big red button is pushed and the building destroyed; the sensitive information within it evaporating.
Similarly, our cells are rigged for self destruction when they become old or defective. The main purpose is to protect the body against replication of defective cells; and to remove old cells.
The program for cellular self-destruction is called apoptosis, which is a type of quality control. The old or defective cells "take one for the team." That some cells die and other live on to replicate helps achieve a balance in the body. If individual cells just replicated and never died, our organs would never cease growing.
What happens in a cancer cell is that some parts of the cell machinery that carry out, signal for, or authorize apoptosis no longer function ... because of damage to genes that produce proteins that regulate or carry out these functions.
Many chemotherapy treatments are designed to exploit apoptosis ... by causing sufficient damage to the cells that force the issue, magnifying the urgency to self-destruct. Waking up the components in the cell that authorize apoptosis, such as the P53 gene.
One way the Rituxan might work is by changing the balance of signals in the cells it binds to to favor apoptosis. Shifting the balance to self destruct without causing damage. (Rituxan may also flag bound cells for destruction by effector cells, which is not dependent on apoptosis.)
Some investigational targeted agents are designed to wake up or silence parts of the cell that carry out or block apoptosis. ...
Imagine that a key protein within the cell is overactive and is giving a STOP order. Then imagine a small molecule drug that fits the shape of this protein, stopping the STOP order. This class of drugs target inhibitors of apoptosis. (Note: If normal cells utilize the same or similar proteins to carry our normal cellular functions, you may have side effects.) ~ KarlS
attenuated - no longer capable of causing infection, as in an attenuated virus to make a vaccine. Also means weakened.
autoantibody - an antibody that reacts against the body's own tissue.
autoimmune disease - a disease that results when the immune system mistakenly attacks the body's own tissues. Examples: Rheumatoid arthritis, systemic lupus erythematosus, and type 1 diabetes.
b-cells (also called B lymphocytes) - a type of white blood cells that come from bone marrow and develop into plasma cells, mature B cells capable of producing antibody. Each b-cell is capable of making an antibody specific to the triggering antigen. The antigen trigger causing it to produce numerous plasma cells capable of manufacturing the antibody.
biological marker (biomarker): A characteristic that is objectively measured and evaluated as an indicator of normal biologic processes, pathogenic processes, or pharmacologic responses to a therapeutic intervention. www.fda.gov/cder/guidance/6400fnl.pdf
bronchi - airways in the lungs
CD (clusters of differentiation)- As b-cells mature, they express different protein receptors on their surface. Some of these receptors can be used as treatment targets. These proteins or antigen markers are called Clusters of Differentiation (CD).
cell - building block that makes up tissues, organs, systems, and blood of the body.
chemokines are molecules released by pathogens and infected tissues that attract lymphocytes
chromosome - physical structure in a cell that contains genes. Almost every human cell has 23 pairs of chromosomes.
complement - a series of blood proteins whose action "complements" the work of antibodies. Complement destroys bacteria, produces inflammation, and regulates immune reactions.
complement-dependent cytotoxicity (CDC): A mechanism of killing cells in which antibody bound to the target cell surface fixes complement, which results in assembly of the membrane attack complex that punches holes in the target cell membrane resulting in subsequent cell lysis. Picture it
cytokines are molecules released by cells to alter lymphocyte function.
DNA - Deoxyribonucleic acid - the basic instruction set for the development and activities of cells.
is like a library which contains thousands of books, called genes. DNA exists in all cells except mature erythrocytes. DNA is made up of bases (nucleotides) that are arranged in a specific sequence. The specificity of the sequence accounts for the production of a specific protein.
effector cells perform a specific function in response to a stimulus; usually used to describe cells in the immune system (such as NK- and Cytotoxic T-cells) that are activated to kill a pathogen or a cancer cell. Also see Antibody-dependent Cell-mediated Cytotoxicity above.
etiologies are the causes of disease.
epigenetic refers to the regulation of gene expression - how, when, where, how much, etc.. Two key areas of epigenetic control are and Chromatin Remodeling and DNA Methylation.
epitope refers to the minimal structural unit of an antigen, recognizable for antibodies and lymphocyte antigenic receptors.
familial describes a trait or disease that is observed with higher frequency within the same family, whether the etiology [cause] is genetic or environmental, or a combination of the two. Where a hereditary disease is one that is caused by a genetic trait.
gene - a unit of genetic material that is inherited from a parent. A gene carries the directions a cell uses to perform a specific function, like making proteins. Genes are made of DNA, the basic chemical unit of life. Genes contain the instructions or recipes for the creation (expression) of unique proteins that carry out cellular functions, such as divide, migrate, or die.
germline mutation - a mutation (genetic defect) that is inherited from your parents. Compare with a somatic mutation, which is acquired by chance or by exposure to toxins. The majority of cancers result from somatic mutations.
Graft vs Disease (GvD) - the action of donor cells against the cancer cells following a stem cell translant.
Graft vs Host Disease (GvHD) - a sometimes serious complication of stem cell transplants in which cells from a donor attack organs of the body. Also see GvHD
granulocyte - a cell filled with potent chemicals that destroy germs and reduce inflammation.
hepatitis - a liver disease.
HLA stands for Human Leukocyte Antigens. These proteins are unique markers found on the surface of nearly every cell in the body, and are in especially high concentrations in white blood cells.
histiocytic -connective tissue containing large white blood cells
humoral immunity - mainly involves b-cells, with the cooperation of helper t-cells. Like macrophages, b-cells take in and process antigens recognized as not belonging in the body. Unlike macrophages, a b-cell can bind only to an antigen that matches it's antibody receptor (idiotype). When helper t-cell signals are present the antigen exposed b-cell will multiply, and soon differentiate into plasma cells that create vast quantities of identical antigen-specific antibodies. Released into the blood, the antibodies lock onto matching antigens, which may trigger complement-dependent cytotoxicity (CDC) and/or antibody-dependent cell-mediated cytotoxicity (ADCC).
hypermethylation - [a term describing the activity of genes] can cause oncogenes to produce proteins that cause malignant behavior. Chromatin Remodeling - Protein fibers called histones that interact with DNA. Drugs that inhibit histone deacetylases, for example, may enable expression of tumor suppressor genes.
hyperplasia (hye-per-PLAY-zha) - An abnormal increase in the number of cells in an organ or tissue. (source NCI)
hypomethylation - [ [a term describing the activity of genes] can quiet genes that normally suppress cancer (tumor suppressor genes).
IgA, immunoglobulin A - a type of antibody concentrated in mucous membranes and body fluids like tears, saliva, and secretions of the respiratory and gastrointestinal tract.
IgG, immunoglobulin G - the major antibody found in the blood that can enter tissues. It coats germs, helping other cells to seek and destroy them.
IgM, immunoglobulin M - an antibody that remains in the bloodstream where it can kill bacteria that enter the blood stream.
immunoglobulins - a large family of proteins, also known as antibodies. There are five classes of immunoglobulins: IgA, IgM, IgG, IgD, and IgE. Picture-it
immune response - reactions of the immune system to foreign substances.
immune system - complex network of specialized cells and organs that has evolved to defend the body against attacks by foreign invaders.
immunity - protection from disease-causing microbes or pathogens.
immunization - the process of inducing protection (immunity) against the destructive forces of a disease-causing microbe.
immunoblastic - large lymphocyte that has been stimulated by an antigen
Immunophenotyping: tests that reveal the kinds of surface molecules that are present on cells (typically immune cells), such as CD20, CD22. CDs stand for clusters of differentiation, which show the developmental stage of the cell and the cell type. CD20, for example, is expressed only on mature b-cells, but not t-cells.
Innate immunity (non-specific immunity) - consists of the pre-existing and fast-acting defenses of the body, such as skin, mucous, cilia, cytokines, and other secretions. It may be that innate immunity also emits signals that activate adaptive immunity.
induction therapy typically consists of conventional doses of chemotherapy administered in an attempt to reduce the amount of cancer in a patient’s body prior to high-dose therapy to be followed by a stem cell transplant.
infection - a state in which microorganisms have taken residence and multiplied in body tissues.
inflammation - an immune system reaction to stop the progression of disease-causing microbes, sometimes seen at the site of an injury. Signs of inflamation include redness, swelling, and heat.
leukemogenic* therapies. - * "The risk of leukemia was greatest four or five years after chemotherapy began, and the risk was elevated for at least eight years after the cessation of chemotherapy. The drugs cyclophosphamide, chlorambucil, melphalan, thiotepa, and treosulfan were independently associated with significantly increased risks of leukemia, as was the combination of doxorubicin hydrochloride and cisplatin. Chlorambucil and melphalan were the most leukemogenic drugs, followed by thiotepa; cyclophosphamide and treosulfan were the weakest leukemogens, and the effect per gram was substantially lower at high doses than at lower doses. The extent to which the relative risks of leukemia are offset by differences in chemotherapeutic effectiveness is not known." http://content.nejm.org
lymph nodes - small bean-shaped organs of the immune system, distributed widely throughout the body. They provide an environment where lymphocytes can receive initial exposure to foreign antigens (viruses, bacteria, fungi, etc.). This activates the lymphocytes to perform immune functions. Most lymph nodes form in clusters throughout the system, such as in the neck, armpit, and groin.
lymphocytosis is an abnormal increase in the number of lymphocytes — a type of white blood cell — in your blood. The most common cause is viral infection, such as EBV, CMV, rubella, whooping cough, toxoplasmosis, brucellosis, chronic lymphatic leukaemiam, and leukemic phase lymphoma.
lymphoblastic - immature lymphocyte - white blood cell in early stage of development.
lymphocytes - small white blood cells (B and T cells) that provide immune defense.
neoplasia (NEE-o-PLAY-zha) Abnormal and uncontrolled cell growth. (source NCI)
neutrophils - an important white blood cell that is both a phagocyte and a granulocyte abundant in the blood.
nodular - well-defined knot of tissue
macrophage - a large immune cell that gobbles microbes and presents antigens from the ingested pathogen to other immune cells. To further orchestrate an immune attack, macrophages send protein signals none as monokines.
MHC molecules - At the heart of immunity is the ability of immune cells to distinquish self from none self. So a fundamental question is how do immune cells do this? Is it by shape? Color? Scent?
As it turns out cell-to-cell communication is a touchy/feely thing, and that when immune cells bump into other cells in the night they grope for a specific molecule called the MHC. Your immune cells can tell by feeling for the distinctive structure of this molecule (it's protein signature) if it's one of your own ... so the correct MHC is a password for safe passage in your body. The diversity of the MHC molecule from one individual to another is sometimes referred to as polymorphism, and this diversity that's encoded onto each cell of your body is the reason transplanted tissue is typically rejected.
"One group of proteins encoded by the genes of the MHC are the markers of self that appear in almost all body cells. Known as class I MHC antigens, these molecules alert killer t cells to the presence of body cells that have been changed for the worse - infected with a virus or transformed by cancer - and that need to be eliminated. "
"A second group of MHC proteins, class II antigens, are found on b cells, macrophages and other cells responsible for presenting foreign antigen to helper t cells. Class II products combine with particles of foreign antigen in a way that showcases the antigen and captures the attention of the helper t cells. "
Source: Understanding the Immune System ~ NIH
microbes - bacteria, fungi, or virus that invades the body. Also called a pathogen.
molecule - The smallest physical unit made up of a chemical substance such as a protein or a fat. Molecules are the building blocks of a cell, and a gene determines how each molecule is produced.
mucous membrane - The moist lining of certain body cavities such as the mouth.
mutation - a change in a cell's DNA that may cause the cell to produce an abnormal protein.
methylation - is a hallmark of cancer. Specifically, it is the addition of a methyl group to specific cytosines (the components of DNA) that regulates gene activity.
oncogenes - mutated and/or over-expressed versions of normal genes that can cause a cell to lose growth restraints, fail to differentiate (mature to a next stage), or prevent the cell from initiating the programmed cell death process called apoptosis. Some oncogenes turn on other genes that promote cancer.
opsonization - a process that identifies cells or bacteria to the phagocytic system (immune cells that engulf pathogens) that then and attack and engulf cells or bacteria that have been identified to them by the complement or antibody system.
opportunistic infections - infections caused by microbes that usually do not cause disease in healthy individuals, but which can result in overwhelming and widespread infection in people with immune deficiency.
palliative care - the goal is to achieve the best possible quality of life for patients and their families when the patients disease is not responsive to curative treatment.
pathogen is a disease causing microorganism
phagocytes - large white blood cells that contribute to immune defense by engulfing microbes, such as bacteria and fungi, or other cells and foreign particles.
refractory is resistance to standard treatment.
RNA - In order for DNA to produce a protein, an intermediate step is required. In this step, DNA is transcribed into RNA (messenger RNA, or mRNA). The sequence of mRNA that encodes a protein is oriented in only one direction, which is known as the "sense" orientation.
salvage therapy -- a term often applied to combinations of chemotherapy drugs used to treat lymphomas after relapse in which the patient is either not responsive to standard protocols, or the patient has general health consideration (allergies, lung, or heart problems) that require the use of unusual combinations of treatment agents, dosing or dosing schedules. Be aware that despite the negative connotation of "salvage," these novel treatments regimens can sometime achieve remissions.
somatic mutation - a mutation (genetic defect) which is acquired by chance or by exposure to toxins. The majority of cancers result from somatic mutations. Compare with germline mutations that are inherited from your parents.
stem cell transplant (bone marrow transplant) - the goal of this treatment is to cure the patient with aggressive therapies that partially or completely kills off (ablates) the normal stem cells in the marrow - the spongy tissue found in the cavities of the body's bones, where all the body's blood cells are produced. These cells are then replaced with the patient's own stem cells (harvested prior to treatment), or matched donor cells.
T cells (T lymphocytes) - white blood cells that either orchestrate the immune response (regulatory T cells) or directly attack infected or malignant cells (cytotoxic T cells).
tissue - a group of similar cells joined to perform the same function.
tissue type - the type of histocompatibility antigens on a person's cells or tissues. If the histocompatibility antigens do not match well, there is a much greater chance that the recipient will reject the donated tissue.
titers is a measurement of the concentration of a substance in a solution. It usually refers to the amount of medicine or antibodies found in a patient's blood.
tolerance is a non-reactivity of the immune system to self.
tumor suppressor genes - genes that protect cells from cancer. They may put the brakes on accelerated growth, or initiate cell death when DNA damage is detected. DNA damage. The under expression of tumor suppression genes can lead to malignant behavior.
vaccinal effect - when a therapy leads to recognition of tumor antigens (abnormal proteins) as foreign leading to attack of remaining tumors by t-cells.
vaccine - substance that contains parts of antigens from an infectious microbe. By stimulating an immune response (but not disease), it protects the body against subsequent infection by that organism.
|